- Home
- »
- Healthcare IT
- »
-
Healthcare Reimbursement Market Size, Industry Report, 2018-2026GVR Report cover
![Healthcare Reimbursement Market Size, Share & Trends Report]()
Healthcare Reimbursement Market Size, Share & Trends Analysis Report By Claim (Fully Paid, Underpaid), By Payers (Private, Public), By Service Provider (Hospitals, Diagnostic Labs), And Segment Forecasts, 2018 - 2026
- Report ID: GVR-2-68038-675-2
- Number of Pages: 120
- Format: Electronic (PDF)
- Historical Range: 2014 - 2016
- Industry: Healthcare
Report Overview
The global healthcare reimbursement market size was estimated at USD 3.59 trillion in 2017. Growing healthcare burden on developed and developing economies coupled with favorable regulatory policies and supportive reimbursement scenario has been primary growth stimulants for the market.
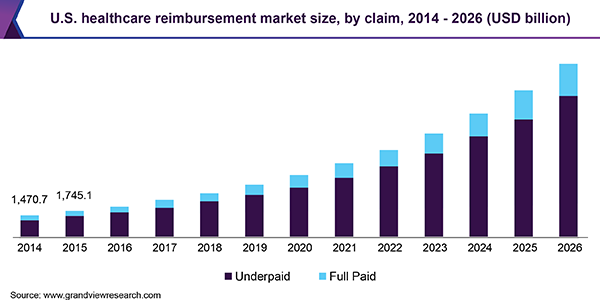
There has been a rise in the healthcare cost in the U.S. as compared to average annual income of the people. The healthcare costs were USD 3.3 trillion in 2016 that equals 17.9% of the gross domestic product. It consumed 6.0% of the overall income in 2013. The U.S. economic distress has increased the burden of healthcare costs on individuals as well as businesses. After introduction of the Obamacare Act, there was a decrease in the out-of-pocket health spending by 12.0% of all citizens in a two-year span.
Growing patient volume along with increased cost of prescription medicine are resulting in a burden on individuals, which is likely to spur the growth of the market. Also, a persistent increase in cost of healthcare is encouraging stakeholder interest in reimbursement. Healthcare spending is increasing because prices for doctor consultation, treatment, and prescription drugs are witnessing upswing.
Changing lifestyles are resulting in rise prevalence of chronic diseases such as heart diseases, diabetes, and cancer, which turn are boosting the healthcare cost. Almost half of the population in America have at least one of these diseases and they are expensive to treat. Improvements in modern medicine augmented the cost of providing healthcare and made it possible to increase the life expectancy of people.
Various initiatives from public and private entities have also been playing a vital role in the development of the market. For instance, the Affordable Care Act (ACA) implemented in the U.S., focuses on expanding health insurance coverage to individuals with low income. The law supports innovative methods to deliver medical care to reduce health care costs and makes affordable health insurance available to more people.
In addition, the model of shifting payment promotes healthcare providers to form accountable care organizations (ACOs) that coordinate care among primary care physicians, hospitals, pharmacists, and other healthcare providers to improve quality of care while reducing costs.
Claim Insights
The underpaid segment accounted for the largest share of the global market owing to increasing number of false claims and unnecessary utilization of healthcare services resulting in underpaid settlements. There are many incidences of defraud of federal and state government health care programs by individuals and businesses. This includes submitting a claim for healthcare treatment, services, medical devices, and pharmaceutical that were never rendered. However, to have control over all the frauds, the False Claim Act was introduced.
Also, individuals are more likely to utilize services when they are not paying the full cost of those services. There are people who intentionally use healthcare services that are not medically required. For instance, some people might visit a physician or a walk-in clinic for the social value of human companionship rather than to address a medical necessity.
Payers Insights
Private payers dominated the market in 2017. They are estimated to remain dominant throughout the forecast horizon owing to the fact that a large number of private players are present in the market. Also, more than 125 health insurance companies provide private health coverage in the U.S.
The Affordable Care Act or Patient Protection and Affordable Care Act (PPACA) is effective since 2014 in the U.S. Health care reform legislations intend to increase the affordability, availability, and use of health insurance. Several provisions in the Affordable Care Act involve an expansion of the private insurance market. It generates incentives for employers to provide health insurance and requires people, not covered by government or employer insurance program, to purchase private health insurance. This factor is, thus, contributing to the growth of the segment.
Service Provider Insights
Hospitals were the leading service providers in the healthcare reimbursement market in 2017. This can be attributed to increasing geriatric population along with rising number of surgeries. Merging hospital systems to cover a large population or geographic area generates more bargaining power to escalate reimbursement.
In North America, hospitals are paid on the basis of diagnosis-related group (DRG) representing fixed amount for every hospital stay. The hospital, treating a patient and spending less compared to DRG payment, makes a profit and when hospitals spend more than DRG payment to treat patients, they lose money.
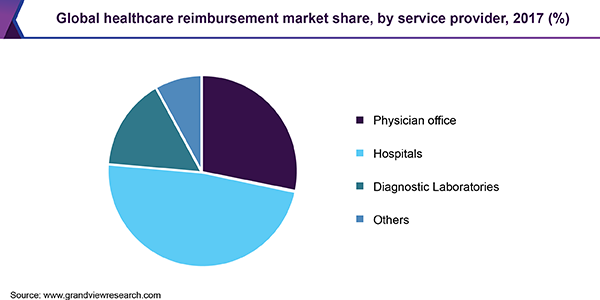
Physician office is anticipated to witness significant growth during the forecast period owing to growing patient pool along with increasing government reforms pertaining to adoption of advanced healthcare infrastructure. Also, contributing on numerous insurance plans indicate that providers have access to a large pool of potential patients, maximum of them benefit from low-cost healthcare coverage under ACA.
Regional Insights
North America dominated the market in 2017. It is projected to remain dominant throughout the forecast period. Presence of strong reimbursement framework and a large number of insurance players are the key trends benefiting the growth of the market. Also, the Affordable Care Act in the U.S. makes its mandatory to have coverage. The states that did not obey were penalized by the federal government. Hence, it acts as a driving force for the regional market.
Europe followed North America in terms of market share. Increasing geriatric population and subsequently rising chronic diseases, such as cardiovascular diseases, respiratory diseases, and atherosclerosis, are driving the market in this region. Over the past decade, Western Europe’s healthcare systems have developed rapidly towards the adoption of performance-based reimbursement structures.
Asia Pacific is poised to experience the fastest growth over the forecast period. The projected rise in geriatric population and the supportive government initiatives in the developing economies are some of the prime factors expected to boost the market’s growth in this region. Also, the increase in private and public healthcare expenditures, high economic development, penetration of insurance services in rural and urban areas, contribute to market growth.
Healthcare Reimbursement Market Share Insights
The market is highly competitive. Key participants include UnitedHealth Group, Aviva, Allianz, CVS Health, BNP Paribas, Aetna, Nippon Life Insurance, WellCare Health Plans, AgileHealthInsurance, and The Blue Cross Blue Shield Association.In an attempt to retain share, diversify product portfolio, and expand geographic presence, market players are frequently undertaking mergers & acquisitions as their primary strategy.
Healthcare Reimbursement Market Report Scope
Report Attribute
Details
Market size value in 2020
USD 7.2 trillion
Revenue forecast in 2026
USD 20.45 trillion
Growth Rate
CAGR of 19.0% from 2019 to 2026
Base year for estimation
2017
Historical data
2014 - 2016
Forecast period
2018 - 2026
Quantitative units
Revenue in USD million and CAGR from 2018 to 2026
Report coverage
Revenue forecast, company share, competitive landscape, growth factors and trends
Segments covered
Claim, payers, service provider, region
Regional scope
North America; Europe; Asia Pacific; Latin America; MEA
Country scope
U.S.; Canada; U.K.; Germany; China; Japan; Mexico; Brazil; South Africa; Saudi Arabia
Key companies profiled
UnitedHealth Group; Aviva; Allianz; CVS Health; BNP Paribas; Aetna; Nippon Life Insurance; WellCare Health Plans; AgileHealthInsurance; and The Blue Cross Blue Shield Association
Customization scope
Free report customization (equivalent up to 8 analysts working days) with purchase. Addition or alteration to country, regional & segment scope.
Pricing and purchase options
Avail customized purchase options to meet your exact research needs. Explore purchase options
Segments Covered in the ReportThis report forecasts revenue growth at global, regional & country levels and provides an analysis on the industry trends in each of the sub-segments from 2014 to 2026. For the purpose of this study, Grand View Research has segmented the global healthcare reimbursement market report on the basis of claim, payers, service provider, and region:
-
Claim Outlook (Revenue, USD Billion, 2014 - 2026)
-
Underpaid
-
Full Paid
-
-
Payers Outlook (Revenue, USD Billion, 2014 - 2026)
-
Private Payers
-
Public Payers
-
-
Service Provider Outlook (USD Billion, 2014 - 2026)
-
Physician office
-
Hospitals
-
Diagnostic Laboratories
-
Others
-
-
Regional Outlook (USD Billion, 2014 - 2026)
-
North America
-
U.S.
-
Canada
-
-
Europe
-
U.K.
-
Germany
-
-
Asia Pacific
-
Japan
-
China
-
-
Latin America
-
Brazil
-
Mexico
-
-
Middle East & Africa
-
South Africa
-
Saudi Arabia
-
-
Frequently Asked Questions About This Report
b. The global healthcare reimbursement market size was estimated at USD 6.1 trillion in 2019 and is expected to reach USD 7.2 trillion in 2020.
b. The global healthcare reimbursement market is expected to grow at a compound annual growth rate of 19.0% from 2018 to 2026 to reach USD 20.5 trillion by 2026.
b. North America dominated the healthcare reimbursement market with a share of 59.0% in 2019. This is attributable to the presence of a strong reimbursement framework and a large number of insurance players.
b. Some key players operating in the healthcare reimbursement market include UnitedHealth Group, Aviva, Allianz, CVS Health, BNP Paribas, Aetna, Nippon Life Insurance, WellCare Health Plans, AgileHealthInsurance, and The Blue Cross Blue Shield Association.
b. Key factors that are driving the market growth include increasing cost of healthcare, and supportive government programs.
Share this report with your colleague or friend.
![gvr icn]()
NEED A CUSTOM REPORT?
We can customize every report - free of charge - including purchasing stand-alone sections or country-level reports, as well as offer affordable discounts for start-ups & universities. Contact us now
![Certified Icon]()
We are GDPR and CCPA compliant! Your transaction & personal information is safe and secure. For more details, please read our privacy policy.
We are committed towards customer satisfaction, and quality service.
"The quality of research they have done for us has been excellent."