National Health Data Platforms in the Middle East: From Fragmented Systems to Unified Patient Records
For decades, healthcare infrastructure across the Middle East grew around large hospital campuses-architectural landmarks that signalled national ambition and modern capacity. The region successfully scaled clinical care, emergency units, and specialty hospitals at a pace unmatched across emerging markets. But the foundation of future readiness is no longer concrete or bed counts. It is clinical intelligence, system connectivity, and unified patient records delivered at national scale.
The region-wide acceleration of Electronic Health Records (EHRs) reflects this structural transition. Ministries of health and national digital health authorities have recognized a fundamental truth: without standardized digital patient records, healthcare networks remain operationally strong but clinically blind across facilities. The next phase of transformation is centred on system-level memory-EHRs that talk, learn, validate, and travel with patients across care nodes.

Regional Market Context - Public Platforms Driving National Records
The Middle East has deployed multiple government-owned unified health record programs that now define digital care delivery in the GCC and wider Middle East:
-
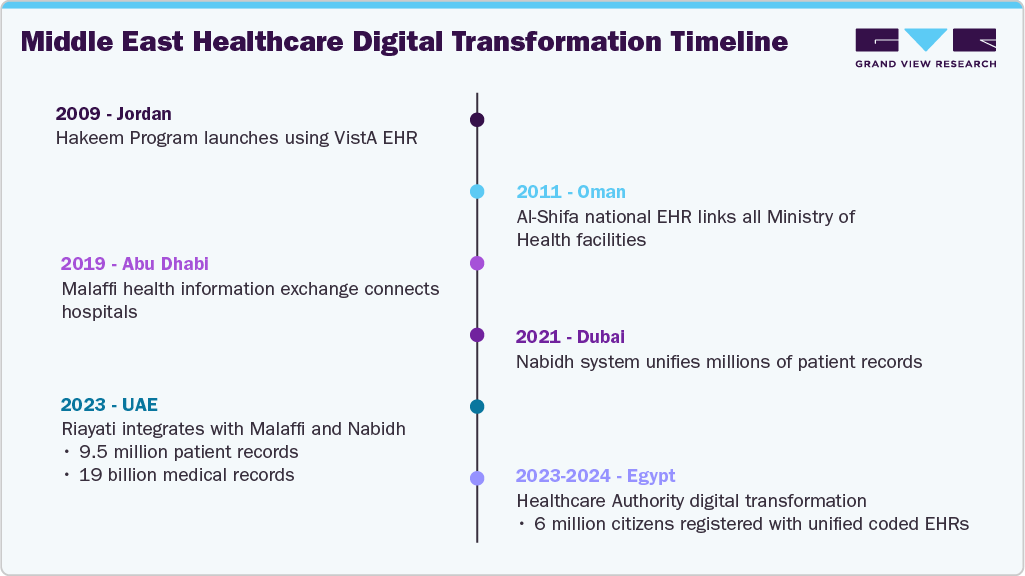
United Arab Emirates (UAE) - The Ministry of Health and Prevention (MOHAP) integrated the national Riayati platform with Abu Dhabi's Malaffi and Dubai's Nabidh systems in 2023. The unified network contains 1.9 billion medical records for 9.5 million patients and is accessible to over 90,000 health providers across 3,057 facilities. The integration's scale demonstrates that the UAE now has a single national medical record accessible in real time.
-
Abu Dhabi (Malaffi) - Launched in 2019 as the region's first health information exchange, Malaffi now stores 3.5 billion clinical records representing 12.7 million unique patients. As of August 2025 it supports 53,476 authorised users across 3,072 healthcare facilities. By 2021 every public and private hospital in Abu Dhabi was connected, enabling more than 39,600 clinicians in 1,539 facilities to access patient information from 98.0% of patient episodes. During the pandemic it managed 63 million PCR tests and about 10 million vaccination records.
-
Dubai (Nabidh) - The Dubai Health Authority reports that its Nabidh platform has unified over 9.47 million patient records and connects more than 1,300 healthcare facilities. Around 81.0% of Dubai's healthcare professionals are actively connected to the system wam.ae wam.ae, ensuring continuity of care across public and private hospitals.
-
Jordan (Hakeem) - The Hakeem program, launched in 2009 under the patronage of King Abdullah II, implements the VistA EHR across public hospitals. By August 2024 the project had digitalised 285 health facilities and aimed to digitalise all public hospitals by the end of 2024. Adoption extends to patient-facing services: The My Hakeem mobile app had 187,206 users from the Ministry of Health and 27,457 from Royal Medical Services; it processed 49,771 medicine deliveries and had 2,647 users booking follow up appointments.
-
Oman (Al Shifa/Shifa) - Oman's Ministry of Health launched the Al Shifa national electronic health record in 2015, linking patient files across government facilities using a unified civil number. The Shifa app acts as a central hub with 16 services, allowing clinicians to follow up on patients and residents to book appointments, access lab results and consult virtually. A 2023 report via the Oman News Agency stated that 172,279 people had registered for the Shifa application since its launch in December 2021
Collectively, these programmes show that the GCC and neighbouring countries are moving beyond pilot projects. Several have already achieved near‑universal connectivity across public hospitals and are extending integration to private providers, primary care centres and even national insurance systems.
Key Drivers of Connected EHR Adoption
1. National digital identity and record portability
Countries across the GCC have paired EHR modernization with national identity rails. UAE health services plug into UAE PASS for secure patient authentication, driving rapid clinician onboarding and medical file linking. Saudi’s NPHIES creates interoperable health files across Cardiac Centers, Dental complexes, labs, and blood banks under Vision 2030. Jordan’s Hakeem platform standardizes national patient files across government hospitals.
2. Ministry-led EHR mandates
Jordan’s Ministry of Health has operationalized the country's largest EMR network using the Hakeem Program (VistA-based). Bahrain’s Ministry of Health launched its national medical file access via the Riayati platform. Government-run systems from UAE’s Nabidh and Malaffi unify patient journeys across public + private hospitals under national digital records.
3. Public health learnings post-pandemic
The pandemic created urgency for digital clinical documentation, immunization logs, lab test tracking, and teleconsultation records to be centralized at population scale. UAE’s digital systems such as Nabidh supported longitudinal clinical record linking of more than a thousand facilities. Saudi’s NPHIES scaled structured digital infrastructure across specialty care nodes including Cardiac, dental, labs, and breast cancer centers.
Key Challenges in the Middle East:
Despite notable progress, the region faces several hurdles:
1. Legacy system fragmentation
Healthcare delivery expanded faster than digital standardization. Many hospital groups still operate mixed HIS + legacy EMRs, now integrating into national solutions like Malaffi and Nabidh.
2. Interoperability gaps between vendors
Even within national HIE ecosystems, different hospital groups historically procured unconnected EMR stacks. Governments have forced consolidation through national medical file utilities:
-
UAE’s Nabidh enforces healthcare system connectivity.
-
Abu Dhabi’s Malaffi mandates hospital-level interoperability.
-
Bahrain’s Riayati unifies national records.
3. Data residency and sovereignty mandates
Regulatory authorities mandate that patient records remain in the country PHI enclave or domestic cloud. UAE, Saudi, Qatar, Jordan and Bahrain enforce national medical file mandates over vendor choices.
4. Workforce readiness and clinician-level transformation
Large-scale EHR rollouts require clinician onboarding, data documentation best practices, structured forms, ICD-based coding, and AI-driven validation into EHRs. Saudi’s platforms emphasize specialty nodes digitization and clinician readiness without hospital-only reimbursements.
Solution framework
EHR adoption in the Middle East is not just about installing software in hospitals. The real transformation comes when healthcare systems ensure that patient records:
-
Move between hospitals, clinics, labs, and pharmacies without breaks
-
Stay inside the country’s protected data environment as required by law
-
Can be used easily by doctors and patients at every care point
-
Are accurate, structured, and consistently updated
The region has built national record platforms to support this:
-
Dubai’s Nabidh connects patient files across 1,300+ facilities and 81%+ of clinicians- one medical record object
-
Abu Dhabi’s Malaffi connects 100% of public + private hospitals - shared clinical history
-
Saudi Arabia uses NPHIES to connect specialty hospitals and care nodes into a unified national health file
-
Jordan’s Hakeem digitized national patient records using VistA
-
Bahrain’s Riayati provides medical history + encounters for citizens + residents
These platforms have shifted the region from system deployment to patient file deployment.
Key principles for a strong EHR strategy
-
National EHR platforms are the central medical data system
- Hospitals must integrate with platforms like Nabidh, Malaffi, NPHIES, Hakeem, Riayati
-
Interoperability is the main requirement
- If systems can’t share records, they create clinical blind spots
-
Data residency is mandatory
- Patient data must stay within national cloud or PHI-protected environments
-
Workforce readiness is critical
- Doctors need structured forms, coding standards, and training
-
Patient record accuracy matters more than UI features
-
Clean and structured data - fancy dashboards
-

The Path Forward
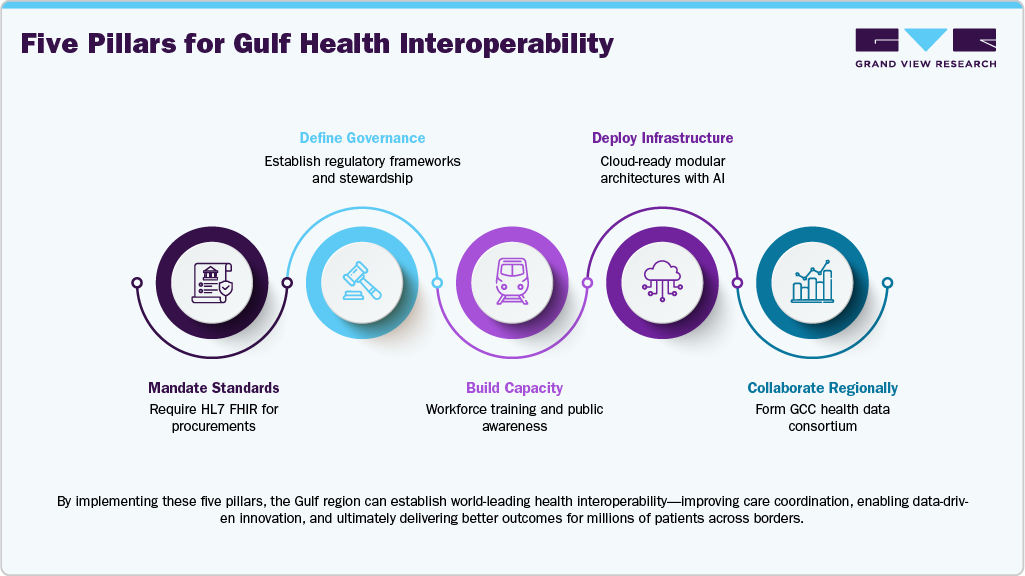
The Middle East’s journey toward EHR adoption is moving from vision to scale, anchored by national health data platforms across the GCC and wider region. Dubai’s Nabidh has connected thousand facilities, while Abu Dhabi’s Malaffi, governed by the Department of Health – Abu Dhabi, ensures unified patient-file exchange across all hospitals. Jordan’s Hakeem and Oman’s Al Shifa demonstrated early nationwide record modernization on open-source-based EHR architectures paired with patient-facing apps. As digital networks expand, integration depth, data sovereignty, clinician readiness, and healthcare-grade security-not system count-will determine resilience. The region’s next decade belongs to connected patient memory, distributed care nodes, and trusted, interoperable, in-country health files.