Robotics in the Middle East: From Early Adoption to Global Healthcare Leadership
The Middle East is experiencing significant transformation in healthcare delivery, establishing itself as a key architect of next-generation robotic medicine. Moving beyond selective technology adoption, the region has rapidly become a hub for advanced robotic-assisted surgery, tele-robotics, and digitally integrated clinical care.
Governments, healthcare systems, and technology partners across the Gulf and Middle East are aligning strategic national visions with practical clinical implementation. This coordinated approach has supported a strong healthcare robotics ecosystem, delivering measurable patient outcomes while setting new standards for efficiency, scalability, and clinical sophistication.
The Evolution of Surgical Robotics in the Middle East
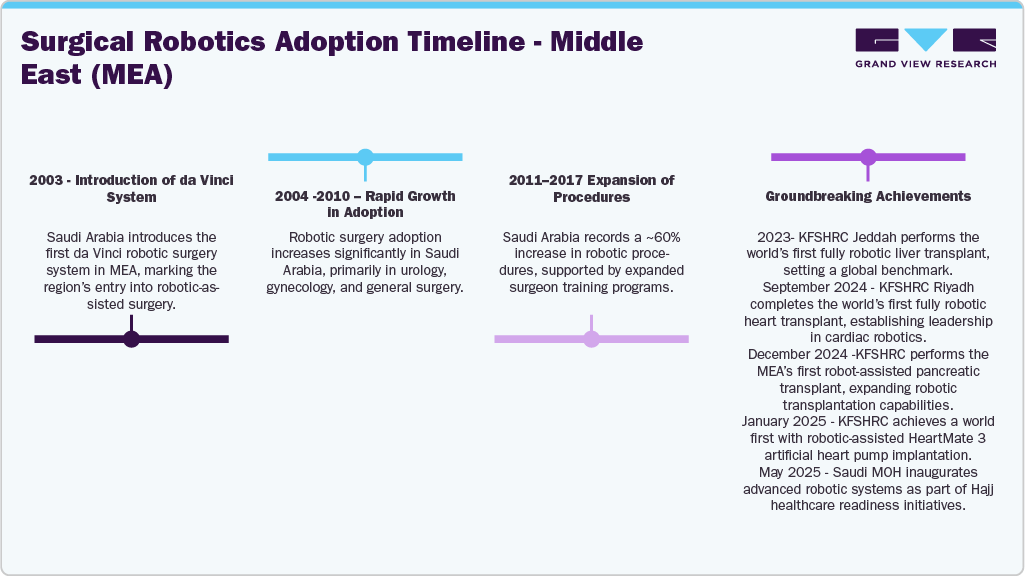
The Middle East’s adoption of surgical robots has progressed rapidly from early 2010s pilots in tertiary hospitals primarily in urology and minimally invasive procedures to multi-specialty integration across cardiology, oncology, bariatrics, gynecology, orthopedics, and complex abdominal surgeries. Post-2020, adoption accelerated due to system resilience needs, workforce constraints, case complexity, and focus on precision outcomes. Leading institutions now embed robotic platforms into routine workflows, signaling a shift from technology acquisition to long-term capability building. Saudi Arabia’s timeline exemplifies this evolution from experimentation to global clinical leadership.
Advancing Clinical Frontiers Through Robotic Integration
Leading hospitals across the Middle East are demonstrating how robotics can fundamentally reshape clinical practice.
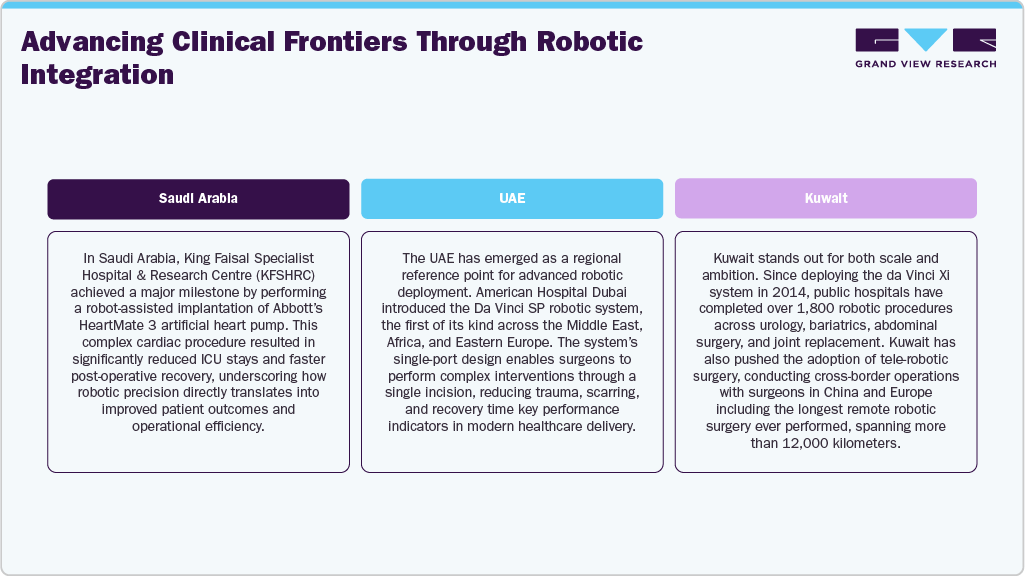
These examples collectively illustrate a critical transition: robotics is no longer confined to centers of prestige it is becoming an operational backbone of advanced care delivery.
Forces Shaping the Region’s Rapid Robotics Adoption
-
Scaling Demand for Robotic Surgery: Rising surgical volumes across cardiology, oncology, urology, bariatrics, and gynecology are accelerating demand for precision-led, minimally invasive robotic procedures.
-
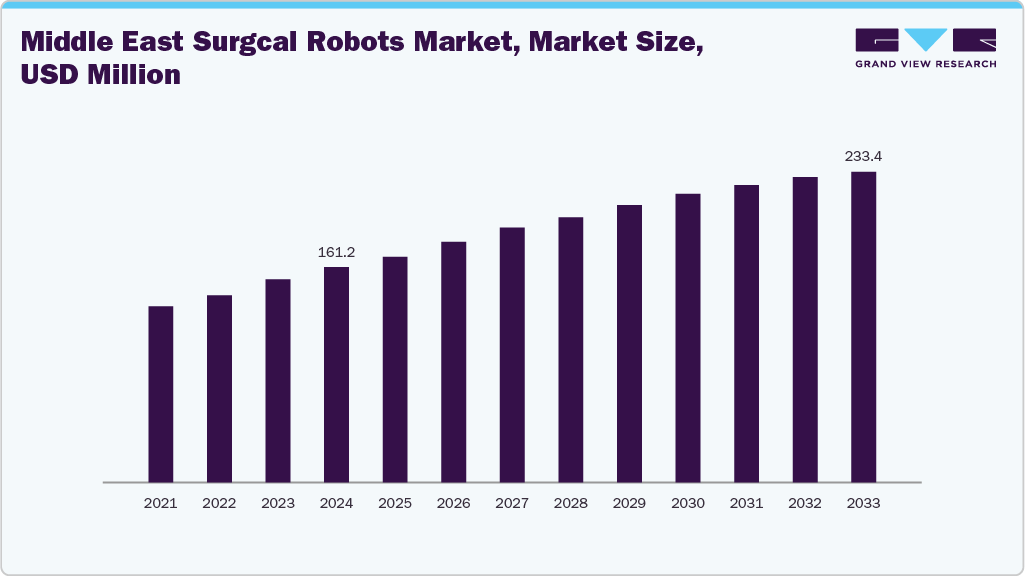
Surgical Robotics Market Expansion: The Middle East surgical robots market is projected to reach USD 233.39 million by 2033, growing at a significant CAGR between 2025 and 2033. This growth is driven by increasing operating room automation, broader adoption of multi-specialty robotic platforms, and the standardization of robotics across hospital systems.
-
Surgical Workforce Constraints: Limited availability of highly specialized surgeons is accelerating robotics adoption to improve consistency and extend surgical capacity. For instance, as of December 2024, American Hospital Dubai, accredited in 2020 by the Surgical Review Corporation (SRC) as the UAE’s first private Center of Excellence in Robotic Surgery, had completed over 1,800 robotic procedures across multiple specialties.
-
Shift Toward Minimally Invasive Care Models: Hospitals are leveraging robotics to reduce length of stay, lower complication rates and enhance recovery. For instance, since launching its robotic surgery program in mid-2022, Dubai Hospital has completed over 145 successful robotic procedures as of October 2025.
-
Digital Hospital Readiness: Leading institutions have built the digital backbone required for advanced robotics. For instance, in November 2024 Sheikh Shakhbout Medical City (SSMC), part of PureHealth and a leading UAE hospital for complex care announced that it has completed 500 robotic-assisted surgeries since launching its program in 2020, including over 200 procedures in 2024.
National Pathways Accelerating Robotic Healthcare in the Middle East
United Arab Emirates (UAE): Systematic Scaling of Robotic Surgery
The UAE has built one of the region’s most structured ecosystems for robotic healthcare deployment, moving from pilot adoption to scaled implementation. National healthcare strategies prioritize robotic-assisted surgery as a core capability, particularly in high-acuity and minimally invasive procedures.
Leading institutions such as Cleveland Clinic Abu Dhabi and American Hospital Dubai have integrated robotic platforms across cardiology, urology, gynecology, and complex abdominal procedures. These deployments are supported by national frameworks that enable procurement, surgeon training, and operational standardization ensuring robotics is embedded into routine surgical pathways rather than limited to showcase cases.
Government-backed initiatives such as the Dubai Robotics & Automation Program (launched 2024, targeting 200,000 robots by 2032 including healthcare applications to boost efficiency) and UAE Artificial Intelligence Strategy 2031 (integrating AI/robotics into healthcare via Dubai Health Authority's Innovation strategy) further reinforce long-term scalability by supporting robotics infrastructure, workforce readiness, and public–private collaboration. The UAE’s approach emphasizes clinical outcomes, operational efficiency, and regional training leadership, positioning the country as a reference market for robotic surgery adoption.
Saudi Arabia: Robotics as a Cornerstone of Advanced Surgical Care
Saudi Arabia represents the most advanced example of robotics-led clinical transformation in the Middle East. Under Vision 2030, robotic surgery has become a strategic pillar of healthcare modernization, with a clear focus on complex, high-impact procedures.
Institutions such as King Faisal Specialist Hospital & Research Centre (KFSHRC) have moved beyond conventional robotic use into world-first fully robotic procedures, including liver, heart, pancreatic transplants, and robotic-assisted artificial heart pump implantation. These milestones reflect a deliberate national strategy to push robotics into the most demanding surgical domains.
Qatar, Kuwait, Bahrain, and Oman: Expanding Regional Capability
Across the wider GCC, robotics adoption is progressing through targeted investments in tertiary care and national referral hospitals.
-
Qatar established the Qatar Robotic Surgery Centre (QRSC) as an early regional hub, enabling multi-specialty robotic procedures and structured surgeon training.
-
Kuwait has emerged as a regional pioneer, performing thousands of robotic-assisted procedures and advancing tele-robotic surgery, including cross-border operations supported by advanced connectivity.
-
Bahrain has incorporated robotic systems into select healthcare facilities, particularly for minimally invasive and precision-driven interventions.
-
Oman is gradually integrating robotic surgery into its hospital modernization efforts, with a focus on improving surgical accuracy and reducing patient recovery time.
These countries collectively contribute to a distributed but strengthening robotics ecosystem, expanding access while building regional surgical expertise.
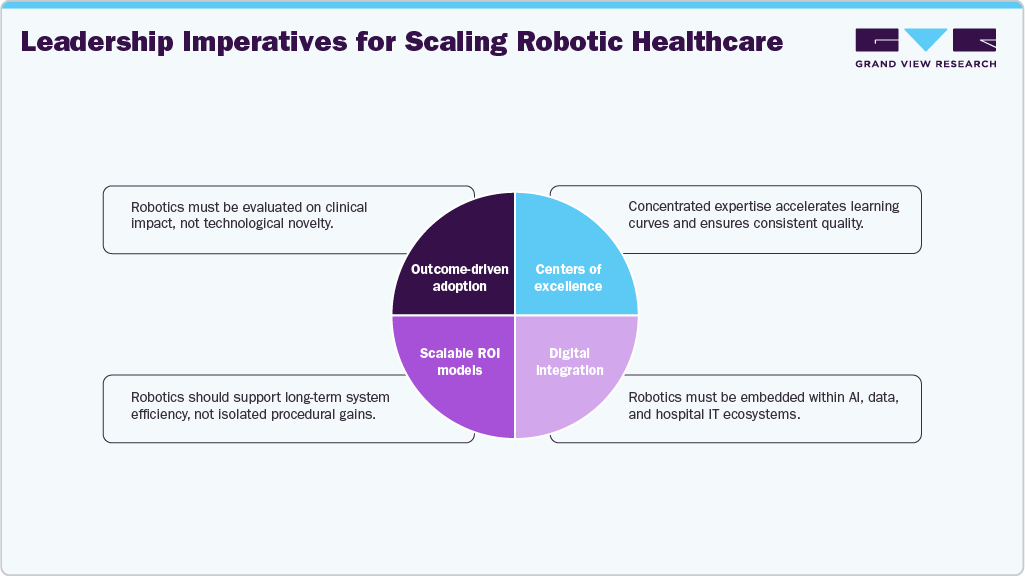
Leadership Imperatives for Scaling Robotic Healthcare
For healthcare leaders, the Middle East’s experience offers several critical imperatives:
The Road Ahead: Building a Robotics-Enabled Healthcare Ecosystem
The Middle East’s robotics journey is evolving from adoption to global leadership in healthcare innovation. Countries in the region are integrating AI-driven analytics, multi-specialty robotic platforms, and advanced digital infrastructure to create seamless, data-informed surgical pathways.
Key strategic directions and future implications for healthcare leaders:
-
Operational Scaling & Coverage Expansion: Robotic surgery adoption is increasingly supported by national policies and insurance frameworks. In the UAE, efforts by the Ministry of Health and private institutions such as Mediclinic City Hospital are expanding insurance coverage for laparoscopic procedures, with robotic surgeries expected to follow, improving accessibility for patients.
-
Global Accreditation & Quality Benchmarking: Hospitals such as Al Qassimi Hospital in Sharjah are achieving Joint Commission International (JCI) accreditation, becoming centers of excellence for complex procedures including robotic cardiac surgery. This elevates UAE’s position in global healthcare rankings and establishes a blueprint for other nations in the region.
-
Precision & Patient Outcomes: Robotics combined with AI-driven surgical planning enhances procedural accuracy, reduces complications, shortens recovery times, and contributes to better patient satisfaction metrics.
-
Workforce Optimization & Capability Building: Training programs and multi-specialty robotic platforms reduce reliance on limited specialized surgeons, improve team efficiency, and support cross-institutional collaboration, including tele-robotics.
-
Strategic Leadership & Ecosystem Development: The UAE is a reference point, achieving top positions in international competitiveness studies, operational excellence, and advanced procedural metrics. By emphasizing robotics, the Ministry of Health is driving a qualitative transformation in healthcare delivery, fostering long-term clinical leadership, and setting regional benchmarks.