- Home
- »
- Medical Devices
- »
-
U.S. Group Health Insurance Market, Industry Report, 2030GVR Report cover
![U.S. Group Health Insurance Market Size, Share & Trends Report]()
U.S. Group Health Insurance Market (2025 - 2030) Size, Share & Trends Analysis Report By Plan Type (HMO, PPO, POS, HDHP/SO), By Firm Size (Small Firm, Large Firm), By Region (Northeast, Midwest), And Segment Forecasts
- Report ID: GVR-4-68040-041-6
- Number of Report Pages: 100
- Format: PDF
- Historical Range: 2018 - 2024
- Forecast Period: 2025 - 2030
- Industry: Healthcare
- Report Summary
- Table of Contents
- Segmentation
- Methodology
- Download FREE Sample
-
Download Sample Report
U.S. Group Health Insurance Market Trends
The U.S. group health insurance market size was estimated at USD 1.41 trillion in 2024 and is projected to grow at a CAGR of 2.2% from 2025 to 2030. The increasing demand for group health insurance, known as employer-sponsored insurance, and its rising average premium price have led to a substantial growth of the market. Additionally, the increasing costs associated with healthcare services and supplies, alongside various government initiatives aimed at improving public health, significantly contribute to the growing demand for group health insurance. These factors create a multifaceted environment where consumers are more frequently seeking medical services and support, leading to a heightened group health insurance market in the U.S.
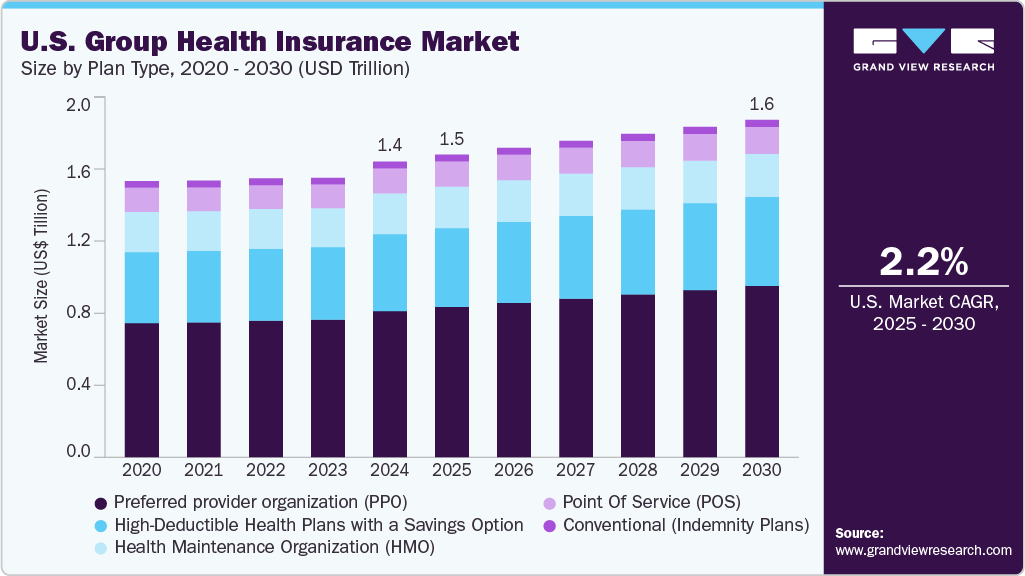
As per the 2024 KFF Employer Health Benefits Survey, rising premium costs significantly drive the overall market, with averages reaching USD 8,951 for single coverage and USD 25,572 for family coverage. These high costs create financial pressure on both employers and employees, prompting companies to seek ways to manage and contain these expenses. Hence, many employers are considering strategies such as shifting more costs to employees, which may include increased deductibles or copayments, or adopting high-deductible health plans with savings options (HDHP/SOs). Currently, 27% of insured workers are under these plans, reflecting a shift towards models that place more financial responsibility on individuals.
Furthermore, the high demand of Preferred Provider Organizations (PPOs) and HDHP/SOs-covering 48% of insured workers demonstrates a market preference for insurance models that offer flexibility and the potential for cost savings. Overall, rising premiums and the increasing adoption of flexible health plans are shaping the future landscape of the U.S. group health insurance industry, influencing both employer strategies and employee options.
Year
Single Coverage Premium
Family Coverage Premium
2018
6,896
19,616
2019
7,188
20,576
2020
7,470
21,342
2021
7,739
22,221
2022
7,911
$2,463
2023
8,435
23,968
2024
8,951
25,572
Moreover, the market is significantly influenced by the employment landscape, particularly regarding small businesses. According to the Commonwealth Fund report published in December 2024, approximately 36 million individuals were employed by private companies with fewer than 50 employees in 2023. This demographic represents a substantial portion of the workforce, yet it is important to note that while small businesses outnumber large corporations, most American workers are still employed by larger firms. One critical aspect of this employment structure is the access to health insurance.
In addition, data indicates that around 49% of employees at small firms have access to health insurance coverage. This contrasts sharply with large employers, where about 98% of employees in companies with 50 or more workers receive health benefits. The disparity in health insurance provision between small and large employers highlights a significant gap in the market.
Characteristics of Private Employer-Sponsored Health Insurance Coverage for Small and Large Firms in the U.S., 2023
Particular
Small firms (<50 employees)
Large firms (50+ employees)
Number of firms (private sector only)
5,945,103
1,955,696
Number of employees (private sector only)
36,329,887
102,245,862
Offer rate (% of private sector employees working in firms offering health insurance)
49.20%
97.60%
Eligibility rate (% of private sector employees eligible for health insurance at firms that offer it)
79.40%
78.70%
Take-up rate (% of private sector employees eligible for health insurance that are enrolled in health insurance at firms that offer it)
66.60%
69.20%
Coverage rate (% of private sector employees enrolled in health insurance at firms that offer it)
52.90%
54.40%
Source: The Commonwealth Fund
The growing trend of self-funded health plans among U.S. employers is primarily driving in the industry growth. As per the 2024 KFF Employer Health Benefits Survey, in 2024, 63% of covered workers were enrolled in self-funded plans, where employers assume the financial risk of providing health care benefits to their employees. This approach is particularly prevalent among large firms, with 79% offering self-funded plans, compared to 20% of small firms. The shift towards self-funding is driven by employers' desire for greater control over health care costs and plan design.
In addition, wellness and health promotion programs are shaping the U.S. group health insurance market. Employers are increasingly integrating these programs to enhance employee well-being, boost productivity, and manage healthcare costs. In 2024, a significant majority of large firms (those with over 200 employees) offering health benefits have adopted wellness initiatives:
-
Health Risk Assessments (HRAs): 56% of large firms provided opportunities for employees to complete HRAs, which are questionnaires evaluating lifestyle, stress, and physical health factors.
-
Biometric Screenings: 44% offered in-person health examinations conducted by medical professionals to measure risk factors such as cholesterol, blood pressure, and body mass index.
- Wellness Programs: 79% implemented programs promoting healthy behaviors, including smoking cessation, weight management, and lifestyle coaching.
To encourage participation, many employers have introduced incentive structures:
- Among large firms offering HRAs, 54% utilized incentives or penalties to motivate employees to complete the assessments.
- Similarly, 65% of large firms with biometric screening programs employed incentives to encourage employee participation.
These strategies reflect a broader trend where employers proactively address health issues and chronic conditions within their workforce. By investing in preventive care and wellness programs, companies aim to reduce long-term healthcare expenditures and improve overall employee health outcomes.
Moreover, the plan enrollment and cost-sharing are highly boosting industry growth. Preferred Provider Organizations (PPOs) remain the most prevalent plan type, indicating a continued preference for flexible provider networks. High-Deductible Health Plans with Savings Options (HDHP/SOs) have gained traction, reflecting a shift towards plans that encourage cost-conscious healthcare decisions. This is influencing the group health insurance industry in the country by driving demand for plans that balance cost and flexibility. Employers are increasingly offering HDHP/SOs to manage rising healthcare expenses, while insurers are adapting their offerings to meet the evolving preferences of both employers and employees. The shift towards higher deductibles and cost-sharing mechanisms underscores the need for innovative plan designs that promote value-based care and employee engagement in health management.
Employer-Sponsored Coverage
Category
Details
Impact on U.S. Group Health Insurance Market
Plan Types
- PPOs cover 48% of workers
- HDHP/SOs cover 27%
- HMOs cover 13%
- POS plans 11%
- Indemnity plans 1%
Preference for flexible plans (PPOs) and growth of consumer-driven plans (HDHP/SOs) reflecting cost-conscious healthcare choices.
Average Deductible
USD 1,787 for single coverage (steady from prior year, but 47% higher than 10 years ago)
Higher deductibles encourage employees to be more engaged in healthcare spending decisions, driving demand for value-based care plans.
Cost-Sharing: Coinsurance
59% of workers’ pay coinsurance for hospital admissions, averaging 21% of costs
Increasing coinsurance shifts more cost responsibility to employees, promoting selective use of healthcare services.
Cost-Sharing: Copayments
16% of workers have companions for hospital admissions, averaging USD 343 per admission
Substantial copayments can influence employee healthcare utilization and plan selection.
Out-of-Pocket Maximums
- 14% of workers have limits under USD 2,000
- 24% have limits over USD 6,001
Wide variation in maximum limits impacts financial risk exposure for employees and influences plan attractiveness.
Market Concentration & Characteristics
The industry is experiencing a high degree of innovation, driven by the need for cost savings, improved member experience, and adaptability to changing regulatory landscapes. Innovation such as alternative member cost-sharing plans, such as zero-deductible and dynamic copay plans, are being introduced to encourage members to use high-quality, lower-cost services. Alternative provider payment plans, including reference-based pricing, are also being adopted, offering savings of 10% to 30% for employers. In addition, risk-pooling products, such as group captives and association health plans, are allowing small and medium-sized employers to increase their bargaining power and enjoy benefits typically reserved for larger companies.
The market saw notable consolidations as larger operators sought to expand their reach and capabilities. For instance, in January 2024, Health Care Service Corporation (HCSC) completed its acquisition of The Cigna Group's Medicare Advantage, Medicare Supplemental Benefits, Medicare Part D, and CareAllies businesses. The acquisition is expected to expand HCSC's capabilities and reach, particularly in the growing Medicare segment.
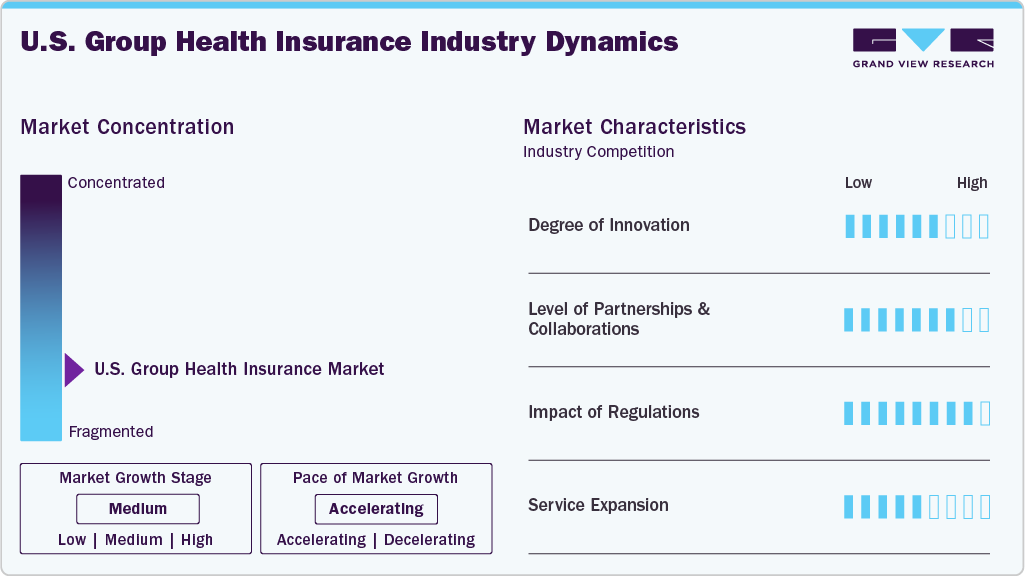
The industry is subject to a complex set of regulations that aim to ensure access to health coverage, affordability, and benefit adequacy. The primary regulatory bodies for group health plans include the Department of Labor (DOL), the Internal Revenue Service (IRS), and the Centers for Medicare & Medicaid Services (CMS). The Affordable Care Act (ACA) has played a significant role in driving the regulatory landscape, introducing provisions such as coverage for pre-existing conditions, extending dependent coverage, and eliminating lifetime and annual limits on essential health benefits. The ACA also established core market rules designed to expand coverage to most people in the U.S., including requirements for premium stabilization and other efforts to protect the risk pool.
Service expansion efforts are evident as companied aim to penetrate underserved markets across the U.S through partnerships and strategic alliances. In April 2025, Sutter Health and SCAN Group have announced a long-term strategic collaboration aimed at enhancing Medicare Advantage (MA) services in Northern California. This partnership planned to introduce new MA products in 2026 and plans to create a new joint venture MA health plan in the near future. The collaboration between Sutter Health and SCAN Group is designed to develop new care models that integrate technology, preventive health strategies, and comprehensive chronic disease management programs.
Plan Type Insights
The PPO plan segment held the largest revenue share of 49.46% in 2024 and is expected to grow at the fastest CAGR over the forecast period. Its dominance is attributed to their flexibility, broader provider network, and lower cost-sharing for in-network services. PPO plans do not require a primary healthcare barrier to screen for specialists and hospital visits, offering lower cost-sharing for in-network services. This flexibility is a significant factor in their popularity, as employees value the freedom to choose their healthcare providers. PPO plans offer a broader provider network compared to other plan types like Health Maintenance Organizations (HMOs). According to the Kaiser Family Foundation's (KFF) Employer Health Benefits 2024 Annual Survey Report, remained the most common plan type, covering 48% of workers.
Plan Type
Single Coverage Premium (USD)
Family Coverage Premium (USD)
HMO
8,218
24,630
PPO
9,383
26,678
POS
8,221
24,164
HDHP/SO
8,275
24,196
KFF Employer Health Benefits 2024 Annual Survey Report
The High-Deductible Health Plans with a Savings Option (HDHP/SO) segment is expected to grow at a significant CAGR over the forecast period. Its growth is attributed to the increasing healthcare costs, which have led employers to seek more cost-effective health insurance options. HDHP/SOs, which typically come with lower premiums but higher deductibles, have become an attractive alternative for employers looking to manage their healthcare expenses. Moreover, the rising trend of consumer-directed healthcare is highly contributing to the growth of HDHP/Sos. This approach encourages employees to take a more active role in their healthcare spending by providing them with more transparency and control over their healthcare expenses. By pairing a high-deductible health plan with a savings option, such as a Health Savings Account (HSA), employees are incentivized to make more cost-conscious decisions about their healthcare.
Firm Size Insights
The large firm segment held the largest revenue share of 92.92% in 2024. Its dominance is attributed to the increasing adoption of group health insurance among large firms, as it serves as a crucial employee benefit and a tool for attracting and retaining talent. Large firms often have more resources to devote to providing comprehensive health insurance to their employees, which can lead to better health outcomes and increased productivity. Large firms dominate the U.S. group health insurance market, with over 90% of large businesses offering health insurance benefits to their employees as large firms recognize the importance of providing comprehensive health insurance as a benefit to attract and retain top talent. Moreover, the regulatory environment also plays a role in driving the demand for group health insurance among large firms. The Affordable Care Act (ACA) requires employers with 50 or more full-time employees to offer health insurance or face penalties, which has led to increased adoption of group health insurance among large firms.
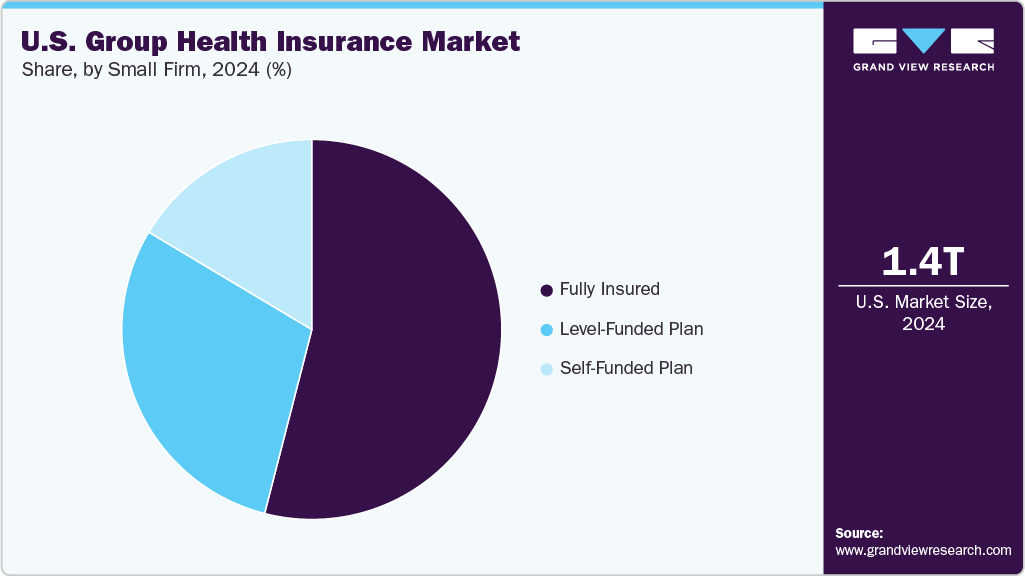
The small firm segment is expected to grow at a lucrative CAGR over the forecast period. Its growth is attributed to the increasing popularity of level-funded plans among small businesses. These plans offer a more predictable cost structure, which can help small firms better manage their health insurance expenses. Moreover, the size of a firm and its industry can significantly impact how sensitive it is to fluctuations in health insurance costs. For instance, smaller firms might have fewer resources to absorb rising insurance premiums, making their financial stability more vulnerable to changes in the market. Furthermore, the average deductible for employees at small businesses tends to be higher than that of larger companies. This distinction can affect employee satisfaction and retention, as higher out-of-pocket costs may deter potential talent from joining or staying with a small firm.
Regional And State Insights
The South region held the largest share of the U.S. market in 2024 due to the presence of noteworthy insurance plans and the substantial population covered by overall group health insurance. In terms of revenue share for the South in 2024, Florida State dominated. The fact that a sizable portion of the population in Florida has employer-sponsored coverage serves as the key supporting evidence. For instance, in Florida, approximately 38% (8.95 million people) of the population had employer-sponsored health insurance in 2023, according to the KFF's insurance coverage data.
Furthermore, the Midwest region continued to hold the second-largest share of the U.S. group health insurance market, with the state of Illinois providing the greatest amount of revenue share in 2024. Over the forecast period, the market will continue to rise due to factors such as group health insurance adoption and cost/benefit analysis.
Key U.S. Group Health Insurance Company Insights
One of the major health insurers in the country is United Healthcare, a division of UnitedHealth Corporation (UHC). For all kinds of enterprises, it provides a menu of group health insurance solutions, including specialty, extra dental, vision, pharmacy, and medical insurance plans. KAISER FOUNDATION GRP, BCBS, and ANTHEM INC GRP are a few of the other providers holding a notable presence in the overall U.S. group health insurance market.
Companies in the U.S. group health insurance market, have been implementing various techniques to retain their clients and expand their market presence. while print advertising isn't completely gone, one of these tactics is digital marketing. To increase market share, having a strong social media presence is invaluable, especially when combined with advertisement on relevant networks, such as Twitter, LinkedIn, etc.
Key U.S. Group Health Insurance Companies:
- Health Care Service Corporation
- Unitedhealth Group
- Kaiser Foundation Health Plan, Inc.
- Blue Cross Blue Shield Association
- Anthem, Inc. (Now Elevance Health)
- The IHC Group
- Health Partners Group Ltd
- Mississippi Insurance Group, LLC
- Providence Health Plan
- Harvard Pilgrim Health Care, Inc.
Recent Developments
-
In March 2025, Transcarent, a digital health platform completed its merger with Accolade, a virtual healthcare and benefits navigation company, in a deal worth USD 621 million. The combined organization will serve over 20 million Members and more than 1,700 employer and health plan clients, providing a comprehensive health and care experience
-
In June 2024, Alliant Insurance Services acquired HMS, a Tampa, Florida-based health insurance agency. HMS focuses on direct-to-consumer ACA plans, combining advanced data science and human expertise to help consumers make informed decisions about their healthcare. The acquisition marked Alliant's continued commitment to under-65 individual health insurance plans.
-
In April 2024, Pivot Health has announced a partnership with Pan-American Life Insurance Group to launch SureCare STM, a proprietary short-term medical insurance product. This product is designed to provide individuals with flexible and comprehensive health insurance coverage options. This partnership is a strategic move to bring innovative health insurance products to the market
U.S. Group Health Insurance Market Report Scope
Report Attribute
Details
Revenue forecast in 2030
USD 1.61 trillion
Growth rate
CAGR of 2.2% from 2025 to 2030
Actual data
2018 - 2024
Forecast data
2025 - 2030
Quantitative units
Revenue in USD million/billion and CAGR from 2025 to 2030
Report coverage
Revenue forecast, company ranking, competitive landscape, growth factors, and trends
Segments covered
Plan type, firm size, region
Regional scope
Northeast; Midwest; South; West
State scope
50 states excluding District of Columbia & Puerto Rico
Key companies profiled
Health Care Service Corporation; Unitedhealth Group; Kaiser Foundation Health Plan, Inc.; Blue Cross Blue Shield Association; Anthem, Inc. (Now Elevance Health); The IHC Group; Health Partners Group Ltd; Mississippi Insurance Group, LLC; Providence Health Plan; Harvard Pilgrim Health Care, Inc.
Customization scope
Free report customization (equivalent up to 8 analysts working days) with purchase. Addition or alteration to country, regional & segment scope.
Pricing and purchase options
Avail customized purchase options to meet your exact research needs. Explore purchase options
U.S. Group Health Insurance Market Report Segmentation
This report forecasts revenue growth, country level and provides an analysis of the latest industry trends in each of the sub-segments from 2018 to 2030. For this study, Grand View Research has segmented the U.S. group health insurance market report based on plan type, firm size, and region.
-
Plan Type Outlook (Revenue, USD Billion, 2018 - 2030)
-
Health Maintenance Organization (HMO)
-
Preferred Provider Organization (PPO)
-
Point of Service (POS)
-
High-Deductible Health Plans with a Savings Option (HDHP/SO)
-
Conventional (Indemnity plans)
-
-
Firm Size Outlook (Revenue, USD Billion, 2018 - 2030)
-
Small Firm
-
Self-Funded Plan
-
Level-Funded Plan
-
Fully Insured
-
-
Large Firm
-
-
Region Outlook (Revenue, USD Billion, 2018 - 2030)
-
Northeast
-
Connecticut
-
Massachusetts
-
Pennsylvania
-
New Jersey
-
New York
-
Others
-
New Hampshire
-
Rhode Island
-
Vermont
-
Maine
-
-
-
Midwest
-
Illinois
-
Indiana
-
Michigan
-
Ohio
-
Wisconsin
-
Iowa
-
Kansas
-
Minnesota
-
Missouri
-
Nebraska
-
Others
-
North Dakota
-
South Dakota
-
-
-
West Group
-
Arizona
-
Colorado
-
Nevada
-
Utah
-
California
-
Oregon
-
Washington
-
Others
-
Idaho
-
Montana
-
New Mexico
-
Wyoming
-
Alaska
-
Hawaii
-
-
-
South
-
Florida
-
Georgia
-
Maryland
-
North Carolina
-
South Carolina
-
Virginia
-
Alabama
-
Kentucky
-
Tennessee
-
Louisiana
-
Oklahoma
-
Texas
-
Others
-
Delaware
-
West Virginia
-
Mississippi
-
Arkansas
-
-
-
Frequently Asked Questions About This Report
b. The U.S. group health insurance market size was estimated at USD 1.41 trillion in 2024.
b. The U.S. group health insurance market is expected to grow at a compound annual growth rate of 2.20% from 2025 to 2030 to reach 1.61 trillion by 2030.
b. The PPO plan segment held the largest revenue share of 49.46% in 2024 and is expected to grow at the fastest CAGR over the forecast period. Its dominance is attributed to their flexibility, broader provider network, and lower cost-sharing for in-network services.
b. Some key players operating in the U.S. Group Health Insurance market include Health Care Service Corporation; Unitedhealth Group; Kaiser Foundation Health Plan, Inc.; Blue Cross Blue Shield Association; Anthem, Inc. (Now Elevance Health); The IHC Group; Health Partners Group Ltd; Mississippi Insurance Group, LLC; Providence Health Plan; Harvard Pilgrim Health Care, Inc.
b. Key factors that are driving the market growth include increasing adoption of group health insurance, increasing government initiatives, and growing awareness of overall health insurance.
Share this report with your colleague or friend.
Need a Tailored Report?
Customize this report to your needs — add regions, segments, or data points, with 20% free customization.

ISO 9001:2015 & 27001:2022 Certified
We are GDPR and CCPA compliant! Your transaction & personal information is safe and secure. For more details, please read our privacy policy.
Trusted market insights - try a free sample
See how our reports are structured and why industry leaders rely on Grand View Research. Get a free sample or ask us to tailor this report to your needs.