- Home
- »
- Medical Devices
- »
-
U.S. Emergency Department Market, Industry Report, 2033GVR Report cover
![U.S. Emergency Department Market Size, Share & Trends Report]()
U.S. Emergency Department Market (2026 - 2033) Size, Share & Trends Analysis Report By Type (Hospital Emergency Department, Freestanding Emergency Department), By Condition, By Service, By Region, And Segment Forecasts
- Report ID: GVR-4-68040-188-8
- Number of Report Pages: 100
- Format: PDF
- Historical Range: 2021 - 2025
- Forecast Period: 2026 - 2033
- Industry: Healthcare
- Report Summary
- Table of Contents
- Segmentation
- Methodology
- Download FREE Sample
-
Download Sample Report
U.S. Emergency Department Market Summary
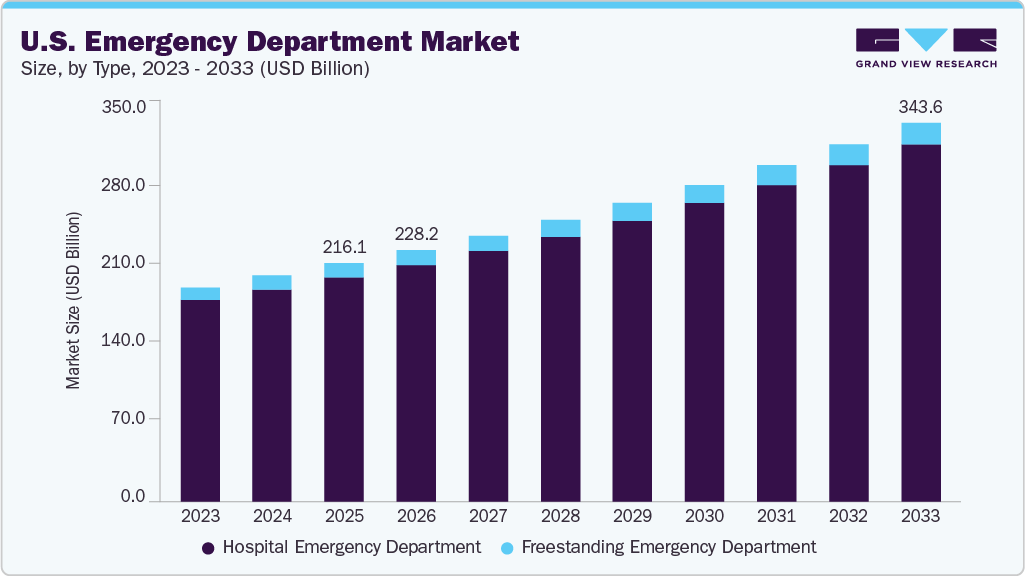
The U.S. emergency department market size was estimated at USD 216.13 billion in 2025 and is expected to reach USD 343.59 billion by 2033, growing at a CAGR of 6.02% from 2026 to 2033. Key market growth drivers include the growing burden of chronic diseases such as cardiovascular conditions, diabetes, and respiratory illnesses, which often lead to acute episodes requiring immediate intervention.
Key Market Trends & Insights
- Based on condition, the infectious segment dominated the U.S. emergency department market with a revenue share of 38.20% in 2025.
- Based on service, the imaging services segment is expected to grow at the fastest CAGR during the forecast period.
- Based on type, the hospital emergency department segment dominated the U.S. emergency department market in 2025.
Market Size & Forecast
- 2025 Market Size: USD 216.13 Billion
- 2033 Projected Market Size: USD 343.59 Billion
- CAGR (2026-2033): 6.02%
In addition, many patients continue to rely on emergency departments as a primary access point due to shortages of primary care providers, limited after-hours services, and barriers to timely outpatient care. Moreover, supportive government initiatives and healthcare policies aimed at improving emergency care infrastructure and reducing patient wait times also drive the market growth.
High Number of Emergency Department Visits:
A high volume of emergency department visits serves as a significant driver for the U.S. emergency department industry, as it directly elevates the demand for emergency care services. The frequent utilization of EDs arising from chronic diseases, acute medical conditions, accidents, and seasonal health fluctuations necessitates the expansion of ED capacity, modernization of facilities, and adoption of advanced diagnostic and treatment technologies. This sustained patient inflow also encourages increased investment in workforce augmentation, including the recruitment of additional emergency physicians, nurses, and support staff, as well as the implementation of operational efficiency solutions, such as electronic health records and triage management systems. Therefore, the consistently high number of ED visits maintains market activity and stimulates growth by compelling healthcare providers to enhance service availability, optimize patient outcomes, and address the rising demand for timely and effective emergency care.
According to the CDC, approximately 140 million emergency department (ED) visits occur in the U.S. each year. Among all adults, the percentage of mental health-related ED visits decreased with increasing age, with 56.3% of visits among adults aged 18-44, 30.1% among adults aged 45-64, and 13.6% among adults aged 65 and over. The majority of the emergency care (about 60%) was provided outside of business hours (other than 8 am to 5 pm), implying that the absence of less expensive alternatives is a significant factor contributing to the high number of ED visits.
Rising Patient Volumes Driven by Demographic and Epidemiological Shifts:
Increasing patient volumes, fueled by demographic changes and rising chronic disease rates, are a key factor driving the growth of the U.S. emergency department industry. As the population ages, more people require frequent and complex medical care, especially older adults with multiple health issues. Chronic conditions such as heart disease, diabetes, and COPD often lead to sudden complications needing urgent attention, most often handled in hospital EDs.
According to a Population Reference Bureau article published in January 2024, the population of Americans aged 65 & older is expected to grow from 58 million in 2022 to 82 million by 2050, representing a 47% increase. In addition, this age group’s proportion of the overall population is anticipated to rise from 17% to 23%. Moreover, the geriatric population in the U.S. is the highest compared to the past. Furthermore, as per a World Economic Forum article published in September 2023, Japan is experiencing a significant aging trend, with over 1 in 10 of its population aged 80 or older. Nearly a third of the population, approximately 36.23 million people, are aged 65 & above. In addition, the number of centenarians in the country is at an all-time high.
Limited Access to Primary and Ambulatory Care:
Many communities continue to face shortages in primary care physicians, long waiting times for appointments, and inadequate behavioral health resources. Hence, patients who cannot access timely outpatient care often turn to emergency departments as their default point of entry into the healthcare system. This includes both individuals with urgent medical needs and those with non-urgent conditions who have no alternative for immediate evaluation. The lack of accessible preventive and routine care also leads to worsening chronic conditions, further increasing the likelihood of ED visits. Therefore, emergency departments experience higher patient volumes, extended wait times, and rising demand for comprehensive diagnostic and treatment capabilities, solidifying EDs as critical safety-net providers within the U.S. healthcare landscape.
According to the MJH Life Sciences report published in May 2025, 1 in 3 minors experiencing a mental health crisis remain in the ED for 12 hours or longer, largely due to appropriate psychiatric beds or specialized inpatient resources are unavailable, particularly in non-children’s hospitals. The study found that 32.1% of pediatric mental health ED visits resulted in prolonged boarding, and that factors such as age, race, and insurance coverage influenced how long children waited for definitive care. These extended stays reflect broader systemic gaps in outpatient and inpatient behavioral health capacity. Hence, EDs are increasingly functioning as holding areas for susceptible children who cannot obtain timely psychiatric evaluation or placement elsewhere, further intensifying ED crowding and heightening operational pressures on hospital emergency departments.
Adoption of Advanced Technologies and Data Analytics:
The growing adoption of advanced technologies and data analytics is a significant growth driver for the market as healthcare facilities increasingly rely on digital solutions to manage rising patient volumes, staffing shortages, and operational inefficiencies. Tools such as AI-enabled triage systems and predictive analytics help EDs anticipate patient surges, prioritize high-acuity cases, and optimize resource allocation, thereby improving clinical outcomes and reducing waiting times. Tele-consultation platforms expand specialist access, enabling faster decision-making for stroke, cardiac, and trauma cases, especially in resource-constrained or rural settings. In addition, real-time operational dashboards allow administrators to monitor capacity, throughput, and patient flow constraints, guiding immediate interventions that enhance ED performance.
Diversification and Care Model Innovation:
The growth of freestanding emergency departments (FEDs) extends emergency services beyond traditional hospital campuses into suburban and previously unserved areas, improving geographic accessibility and reducing travel time for patients. These facilities operate 24/7, are equipped to handle high-acuity cases, and bill at hospital ED rates, thereby generating new revenue streams while capturing unmet demand. Large U.S. hospital systems such as HCA Healthcare, Tenet Healthcare, Ascension, and CommonSpirit Health have aggressively expanded FED networks, particularly in Texas, Florida, Colorado, and Arizona. For instance, in October 2025, HCA Virginia committed nearly USD 60 million to expand emergencies and urgent care access across Central and Northern Virginia, focusing on communities with strong population growth. Under this investment, the health system is expected to build three new freestanding emergency rooms in Richmond, Chesterfield, and Loudoun County which will increase its existing FER footprint from eight to 11 facilities.
Dr. William Lunn, president of HCA Healthcare’s Capital Division said:
“This is about meeting families where they are,” “These new emergency rooms and urgent care clinics are vital community assets that build on the exceptional care we already provide. When every second counts, we want to ensure patients get the help they need - without delay.”
Thus, with the expanding healthcare systems FED networks, overall, ED capacity and utilization increase, directly supporting market growth.
The expansion of observation units within EDs enhances patient and care efficiency by allowing short-term monitoring and treatment without full inpatient admission. This model reduces hospital admissions, lowers costs, and aligns with value-based care goals while still increasing ED service utilization. Observation services also optimize bed management and reimbursement, making ED operations more financially sustainable and attractive for investment.
Moreover, integration of behavioral health services into EDs addresses the rising incidence of mental health crises and psychiatric emergencies in the U.S. By embedding psychiatric assessment, crisis stabilization, and referral services within ED settings, hospitals reduce repeat visits and length of stay while accommodating a growing patient segment. This integration expands the scope of emergency care, increases the complexity of visits, and strengthens the ED’s role as a critical access point for acute behavioral health needs.
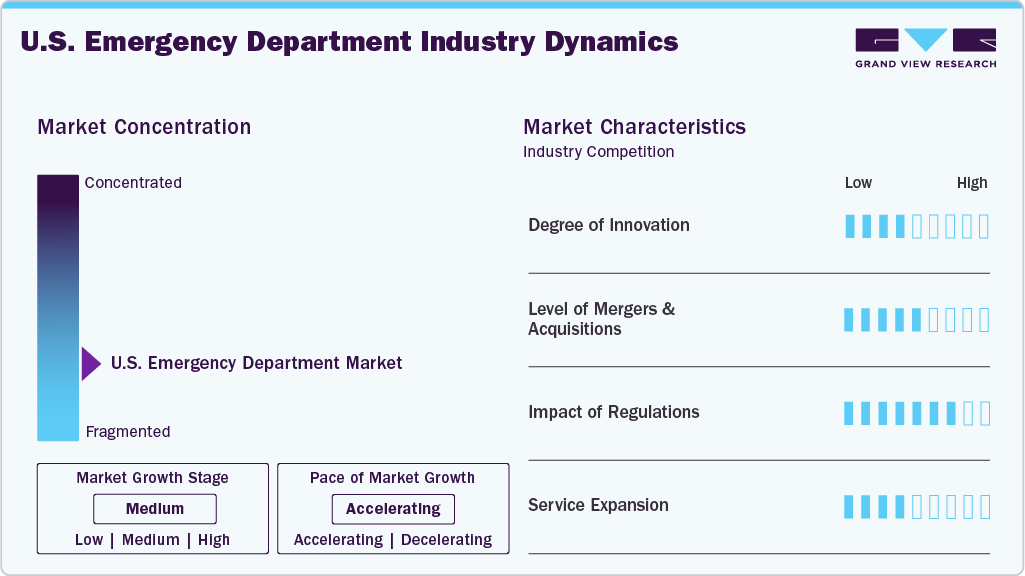
Market Concentration & Characteristics
The U.S. emergency department market is fragmented, with many small players entering the market and launching new innovative products. The degree of innovation is medium, and the level of merger & acquisition activities is medium. The impact of regulations is high on the market and service expansion is medium.
The degree of innovation in the U.S. emergency department industry is high. In September 2025, PointClickCare’s launched its AI-driven Emergency Department (ED) Optimization solution represents a major advancement in real-time clinical intelligence for emergency settings. The platform uses artificial intelligence to deliver instant, actionable insights on patients arriving from post-acute care settings such as skilled nursing facilities, long-term care centers, and rehabilitation sites.
Hamad Husainy, DO, FACEP, chief medical officer, PointClickCare said:
"PointClickCare's AI-informed proprietary Reason for Transfer AI Model is setting a new standard in healthcare intelligence by delivering the critical information emergency departments need instantly," "Often, EDs receive too little data, too late, or an overwhelming amount of unfiltered data, and with this enhanced solution, we are empowering providers with timely, actionable insights that streamline decision-making and elevate patient care."
The market players are leveraging strategies such as partnerships and acquisitions to promote the reach of their offerings and increase their service capabilities. In August 2025, the Emergency Center of Arizona (TEA), a well-established physician-led group managing emergency medicine services across 14 Dignity Health Arizona General Hospital EDs in the Greater Phoenix area (treating approximately 240,000 patients annually), completed a strategic acquisition by Emergency Care Partners (ECP), a national emergency medicine services and ED management provider.
Dr. Keith Butler said:
“What stood out to us about ECP was their commitment to preserving our relationships. Relationships with Dignity, our physician and nursing relationships, and ultimately our patient relationships with their focus on clinical autonomy. Our partnership allows my colleagues and me to continue operating our group in a way that has benefited our patients, physicians, APPs, and hospital partners. It’s a unique partnership that allows local private groups to realize the value of being part of a national team. We’re excited to join a group of like-minded physician leaders who are also owners in ECP and look forward to collaborating with them.”
Regulations play a crucial role in the market, imposing operational standards and care delivery. The Emergency Medical Treatment and Labor Act (EMTALA) mandates that all hospitals with EDs provide medical screening and stabilizing treatment to anyone seeking care, regardless of insurance or ability to pay, making EDs critical safety-net providers. In addition, hospitals are required to comply with Centers for Medicare & Medicaid Services (CMS) Conditions of Participation, which establish requirements for staffing, quality reporting, patient rights, emergency preparedness, and clinical governance.
Market players use a strategy of service expansion to enhance their service capabilities and expand the reach of their offerings. For instance, in August 2025, Emergent Medical Associates officially launched its emergency care services at Kula Hospital, marking a significant enhancement in the hospital’s acute care capabilities. This initiative aims to provide timely, high-quality emergency medical services to the local community, addressing both routine and critical health needs.
Dr. Mark Bell, President of Emergent Medical Associates, said:
“We’re proud to continue expanding our presence in Hawaii with the addition of Kula Hospital,” “Our goal is to deliver clinical excellence and operational efficiency while honoring the culture and community-centered care that defines healthcare in Maui.”
Type Insights
The hospital emergency department segment dominated the U.S. emergency department market in 2025, accounting for the largest revenue share, and is expected to witness the fastest CAGR over the forecast period. This is driven by consistently high patient volumes resulting from the country’s rising burden of acute illnesses, traumatic injuries, chronic disease exacerbations, and mental health crises. Moreover, the growing launch of dedicated, well-equipped emergency wings significantly drives segment growth. For instance, in January 2026, Gleneagles Hospital, Chennai, launched a new, state-of-the-art emergency wing to strengthen acute medical care for the city. The facility is designed to handle a high volume of urgent and critical cases with speed and precision, and includes around 19 beds configured for rapid assessment, triage, resuscitation, and treatment, including a dedicated isolation bed for infection control.
The freestanding emergency department (FSED) segment is anticipated to grow at a significant CAGR during the forecast period. This is driven by rapid suburban population growth and the uneven distribution of hospital-based EDs, which have created demand for convenient, 24/7 emergency access closer to where patients live and work, positioning FSEDs as an effective solution. These facilities reduce travel time, alleviate overcrowding at traditional hospital EDs, and provide timely care for both high-acuity and urgent conditions. From a provider perspective, FSEDs enable hospitals and emergency physician groups to expand their geographic footprint at lower capital cost than building full-service hospitals, while still operating under hospital licensure and billing structures. As per an article published by Clarion Events North America in September 2025, from 2005 to 2019, the number of FSEDs increased by approximately 75%, reflecting a major shift in how emergency services are delivered. Initially developed to reduce overcrowding in hospital-based emergency departments, FSEDs have evolved into standalone, full-service emergency care providers that improve patient access, reduce waiting times, and extend emergency coverage to underserved locations.
Service Insights
The emergency department services segment dominated the U.S. emergency department industry, accounting for a revenue share of 45.86% in 2025. This can be attributed to the wide variety of services available for immediate care. Common medical services include treatment for stomach & abdominal pain, fever, headache, cough, back symptoms, shortness of breath, unspecified pain, throat symptoms, & vomiting. The growth of the segment can be attributed to increasing utilization of data-driven technologies, rising patient footfall in EDs, and growing adoption of Emergency Department Information Systems (EDIS).
The imaging services segment is expected to grow at the fastest CAGR during the forecast period. The segment is experiencing growth due to increased awareness of medical screening to assess the urgency of medical conditions, the prevalence of chronic yet manageable diseases, and the availability of ample economic resources. Furthermore, technological advancements and new product launches by companies are expected to drive the segment during the forecast period. For instance, in October 2023, Philips introduced its Point-of-Care Ultrasound (POCUS) innovations at the 2023 American College of Emergency Physicians Scientific Assembly in Philadelphia, U.S. POCUS technology provides physicians with immediate insight into a patient's condition, expediting care and enabling bedside treatment across various emergency care settings.
Condition Insights
The infectious segment dominated the U.S. emergency department market with a revenue share of 38.20% in 2025, and is expected to grow at the fastest CAGR during the forecast period. Service providers are implementing measures to maintain preparedness to treat infectious diseases, which is propelling segment growth. Medical conditions, such as influenza, pneumonia, Sexually Transmitted Infections (STIs), viral hepatitis, and measles, require emergency medical care. According to a CDC report published in December 2025, Seasonal influenza activity has increased and may continue to increase in most parts of the country in the first week of January 2024.
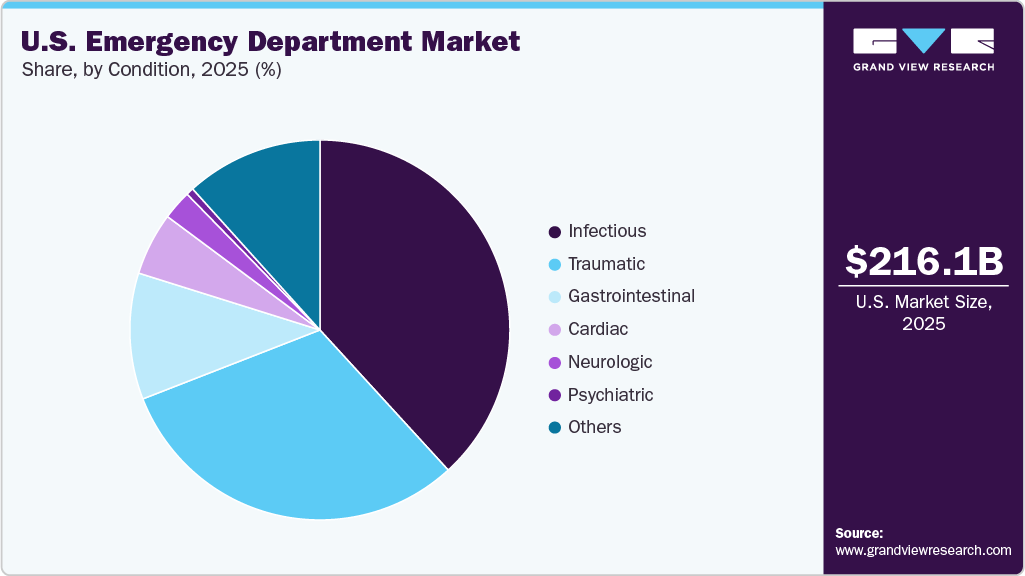
The psychiatric segment is expected to grow at a significant CAGR during the forecast period. Growing rates of anxiety, depression, substance use disorders, and severe mental illnesses, combined with limited access to outpatient behavioral health services, have led to higher ED visit volumes for psychiatric emergencies. Factors such as shortages of mental health professionals, inadequate community-based crisis care, and delayed access to inpatient psychiatric beds further increase ED dependence, resulting in longer patient stays and higher resource utilization.
Region Insights
The Southeast U.S. emergency department market held the largest revenue share of 25.84% in 2025. This can be attributed to rapid population growth, the high prevalence of chronic diseases, and limited access to primary care in many areas. States across the Southeast, such as Florida, Georgia, North Carolina, and Texas, are experiencing strong population growth, including an aging population and retirees, which increases demand for acute and emergency medical services. The region also has higher rates of chronic conditions such as diabetes, cardiovascular disease, and respiratory disorders, leading to more frequent emergency visits.
The West U.S. emergency department industry is expected to grow at a significant CAGR during the forecast period. The region’s vast geography drives this growth, and large rural and frontier areas pose access challenges, making emergency departments, including freestanding emergency departments, critical entry points for acute care. In addition, shortages of primary care providers and limited after-hours care in many Western communities prompt patients toward emergency departments for urgent and non-urgent conditions.
Key U.S. Emergency Department Company Insights
In the U.S. Emergency Department (ED) market, a mix of large health systems, freestanding emergency department operators, and acute care hospital groups plays a leading role in delivering emergency care, shaping market dynamics, and driving expansion strategies. Some of the most influential hospital systems that anchor ED services nationwide include HCA Healthcare, Tenet Healthcare Corporation, Universal Health Services, Ascension Health, Community Health Systems, and Lifepoint Health, which operate both traditional hospital EDs and extensive networks of freestanding emergency departments (FSEDs) to expand access in suburban and underserved regions.
Key U.S. Emergency Department Companies:
Hospital Emergency Departments:
- Parkland Health
- Lakeland Regional Health
- St. Joseph’s Health
- Natchitoches Regional Medical Center
- Schoolcraft Memorial Hospital
- Clarion Hospital
- USA Health
- Baptist Health South Florida
- Montefiore Medical Center
- LAC+USC Medical Center
Freestanding Emergency Departments:
- Tenet Healthcare Corporation
- Universal Health Services, Inc.
- Community Health System
- HCA Management Services, L.P.
- Legacy Lifepoint Health, Inc.
- Ardent Health Services
- Ascension Health
- Deerfield Management Company
- Emerus
- USA Health
Recent Developments
- In January 2026, The American College of Emergency Physicians (ACEP) and several leading national healthcare organizations, including the American Academy of Pediatrics (AAP), the Emergency Nurses Association (ENA), and the American College of Surgeons (ACS), released a joint statement outlining updated, life-saving standards for pediatric readiness in U.S. emergency departments.
Marianne Gausche-Hill, MD, FACEP, FAAP, FAEMS, a statement co-author, said:
“The 2026 assessment is our chance to see where we stand-and where we can do better,” “The NPRP Assessment helps emergency care teams lead efforts to quantify the progress made and improvements needed to optimize emergency care for children. Furthermore, participation in pediatric readiness efforts is among criteria for ACEP’s ED Accreditation (EDAc) program, which demonstrates a commitment to quality and safety.”
- In September 2025, Catholic Medical Center (CMC), part of the HCA Healthcare system, announced and began development of Nashua’s first freestanding emergency room (FSER), marking a significant expansion of emergency care access in southern New Hampshire. The nearly 10,000-square-foot facility at 338 Amherst Street, a former bowling alley site, represents a USD 16 million investment and is slated to open in mid-2026.
John Skevington, chief executive officer of Catholic Medical Center, said:
“Emergencies don’t wait, and neither should patients,” “By expanding access to emergency care in Nashua, we’re ensuring that patients receive fast, expert care for everything from chest pain and stroke to broken bones and abdominal pain. This facility is designed to complement our existing hospitals, physician clinics and urgent care centers by providing another choice when every minute counts.”
-
In December 2025, Children’s Minnesota and the Washburn Center for Children expanded their partnership with the goal of reducing emergency department (ED) boarding, a growing challenge driven by rising pediatric mental health needs. The collaboration aims to provide earlier, more coordinated behavioral health interventions so that children in crisis can access appropriate care faster without prolonged waits in the ED.
“When a child arrives in our emergency room in the midst of a mental health crisis, they are at their most vulnerable. In these critical moments, it is our responsibility to offer not just care, but a lifeline,” said Emily Chapman, MD, president and CEO of Children’s Minnesota. “This partnership is one more step towards supporting families with the tools they need to navigate this difficult journey.”
U.S. Emergency Department Market Report Scope
Report Attribute
Details
Revenue forecast in 2033
USD 343.59 billion
Growth rate
CAGR of 6.02% from 2026 to 2033
Actual data
2021 - 2025
Forecast data
2026 - 2033
Quantitative units
Revenue in USD billion and CAGR from 2026 to 2033
Report coverage
Revenue forecast, company ranking, competitive landscape, growth factors, and trends
Segments covered
Type, service, condition, region
Country scope
U.S.
Key companies profiled
Parkland Health; Lakeland Regional Health; St. Joseph’s Health; Natchitoches Regional Medical Center; Schoolcraft Memorial Hospital; Clarion Hospital; USA Health; Baptist Health South Florida; Montefiore Medical Center; LAC+USC Medical Center; Tenet Healthcare Corporation; Universal Health Services, Inc.; Community Health System; HCA Management Services, L.P.; Legacy Lifepoint Health, Inc.; Ardent Health Services; Ascension Health; Deerfield Management Company; Emerus; USA Health
Customization scope
Free report customization (equivalent up to 8 analysts working days) with purchase. Addition or alteration to country, regional & segment scope.
Pricing and purchase options
Avail customized purchase options to meet your exact research needs. Explore purchase options
U.S. Emergency Department Market Report Segmentation
This report forecasts revenue growth at the country level and provides an analysis of the latest industry trends in each of the sub-segments from 2021 to 2033. For this study, Grand View Research has segmented the U.S. emergency department market report based on type, service, condition, and region:
-
Type Outlook (Revenue, USD Billion, 2021 - 2033)
-
Hospital Emergency Department
-
Freestanding Emergency Department
-
-
Service Outlook (Revenue, USD Billion, 2021 - 2033)
-
Emergency Department (ED) Service
-
Imaging Service
-
Laboratory Service
-
-
Condition Outlook (Revenue, USD Billion, 2021 - 2033)
-
Traumatic
-
Infectious
-
Gastrointestinal
-
Psychiatric
-
Neurologic
-
Cardiac
-
Others
-
-
Regional Outlook (Revenue, USD Billion, 2021 - 2033)
-
West
-
Southeast
-
Southwest
-
Midwest
-
Northeast
-
Frequently Asked Questions About This Report
b. Some key players operating in the U.S. emergency department market include Parkland Health; Lakeland Regional Health; St. Joseph’s Health; Natchitoches Regional Medical Center; Schoolcraft Memorial Hospital; Clarion Hospital; USA Health; Baptist Health South Florida; Montefiore Medical Center; LAC+USC Medical Center; Tenet Healthcare Corporation.
b. The hospital emergency department segment dominated the market with the highest revenue share in 2025 and is expected to witness the fastest growth rate over the forecast period. This is driven by consistently high patient volumes resulting from the country’s rising burden of acute illnesses, traumatic injuries, chronic disease exacerbations, and mental health crises.
b. Key factors that are driving the U.S. emergency department market growth include the growing burden of chronic diseases such as cardiovascular conditions, diabetes, and respiratory illnesses, which often lead to acute episodes requiring immediate intervention.
b. The U.S. emergency department market size was estimated at USD 216.13 billion in 2025.
b. The U.S. emergency department market is expected to grow at a compound annual growth rate of 6.02% from 2026 to 2033 to reach USD 343.59 billion by 2033.
Share this report with your colleague or friend.
Need a Tailored Report?
Customize this report to your needs — add regions, segments, or data points, with 20% free customization.

ISO 9001:2015 & 27001:2022 Certified
We are GDPR and CCPA compliant! Your transaction & personal information is safe and secure. For more details, please read our privacy policy.
Trusted market insights - try a free sample
See how our reports are structured and why industry leaders rely on Grand View Research. Get a free sample or ask us to tailor this report to your needs.