- Home
- »
- Healthcare IT
- »
-
U.S. Healthcare Payers Core Administrative Processing Solutions Market 2033GVR Report cover
![U.S. Healthcare Payers Core Administrative Processing Solutions Market Size, Share & Trends Report]()
U.S. Healthcare Payers Core Administrative Processing Solutions Market (2026 - 2033) Size, Share & Trends Analysis Report By Type (Software, Services), By Deployment (On-premise, Cloud-based), By Region, And Segment Forecasts
- Report ID: GVR-4-68040-304-0
- Number of Report Pages: 90
- Format: PDF
- Historical Range: 2021 - 2024
- Forecast Period: 2026 - 2033
- Industry: Healthcare
- Report Summary
- Table of Contents
- Segmentation
- Methodology
- Download FREE Sample
-
Download Sample Report
U.S. Healthcare Payers Core Administrative Processing Solutions Market Summary
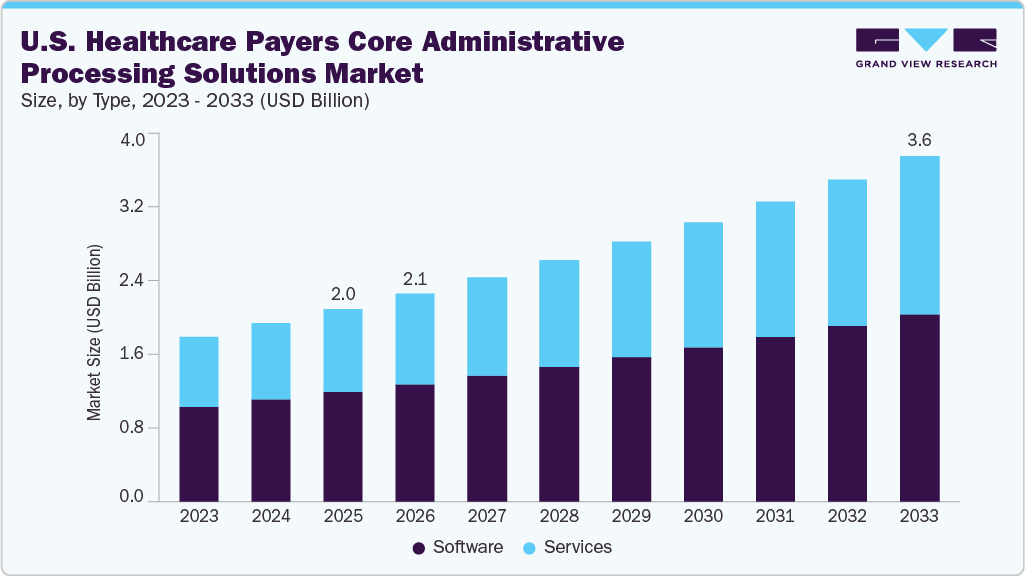
The U.S. healthcare payers core administrative processing solutions market size was estimated at USD 2.0 billion in 2025 and is projected to reach USD 3.6 billion by 2033, growing at a CAGR of 7.5% from 2026 to 2033. The market growth is attributed to the growing demand for cost reduction, technological advancements, the modernization of enrollment and billing processes, the increasing adoption of strategic initiatives by market players, and evolving regulatory and compliance requirements.
Key Market Trends & Insights
- Based on type, the software segment led the market with the largest revenue share of 56.9% in 2025.
- Based on deployment, the cloud-based segment accounted for the largest market revenue share in 2025.
Market Size & Forecast
- 2025 Market Size: USD 2.0 Billion
- 2033 Projected Market Size: USD 3.6 Billion
- CAGR (2026-2033): 7.5%
Modernizing enrollment and billing processes in the U.S. healthcare payers core administrative processing solutions industry is significantly contributing to market growth. By leveraging advanced technologies and streamlined systems, healthcare payers can efficiently onboard new members, ensure accurate billing, and optimize revenue cycle management. This transformation enhances operational efficiency while improving service quality, ultimately driving customer satisfaction and retention. Next-generation core administrative processing solutions (CAPS) provide advanced capabilities that enhance operational efficiency and improve member services. These capabilities deliver significant value to health plans of all sizes, supporting growth and adaptability.-
Hybrid Cloud Delivery
-
Business-Friendly Configuration
-
Adaptable Modern Architecture
-
Ready for Value-Based Models
-
Seamless Ecosystem Integration
Moreover, the adoption of innovative solutions and best practices in enrollment and billing enables payers to strengthen their competitive positioning and achieve sustainable financial performance. For instance, healthcare payers are increasingly adopting AI-driven automation in billing and claims processing, which can reduce labor costs by approximately 35% and lower denial rates by 30-40% in advanced implementations, thereby improving overall accuracy, efficiency, and revenue cycle performance.
Furthermore, the increasing advancements in artificial intelligence have captured the attention of healthcare industry leaders, including health plan executives, solution providers, and academia, regarding its potential effects on healthcare operations. Health payers are implementing AI within core administration processing systems to enhance auto-adjudication rates, streamline prior authorization processes, and mitigate fraud, waste, and abuse.
A study published by the National Bureau of Economic Research in January 2023 found that the broader adoption of AI in healthcare reduces U.S. healthcare expenditures by 5 to 10 percent, translating into annual savings of approximately USD 200 billion to USD 360 billion. The research identifies claims management, member services, and corporate functions as key areas where AI could significantly reduce administrative costs for healthcare payers.
Market Characteristics & Concentration
The market growth is high and accelerating. Prominent players in the U.S. healthcare payers core administrative processing solutions industry are investing in technological advancements in CAPS to meet evolving healthcare regulatory requirements.
The technology solutions in the U.S. healthcare payers core administrative processing solutions industry is characterized by a high degree of innovation, with new technologies being developed and introduced at regular intervals. For Instance, in November 2025, UnitedHealth Group expanded its use of generative AI through its Optum division to automate claims processing and improve care recommendations. This reflects how payers are rapidly integrating AI to reduce costs and enhance decision-making.

Key market players such as Cognizant and HealthEdge Software, Inc., are involved in mergers and acquisitions. These companies are expected to expand their geographic reach and enter new territories through M&A. Similarly, in August 2025, HealthEdge was acquired by Bain Capital in a deal valued at approximately USD 2.6 billion, aimed at strengthening next-generation payer technology platforms and expanding capabilities in AI-driven healthcare solutions.
The country's regulations are primarily aimed at fraud & abuse in healthcare, with the goal of reducing provider misconduct and recovering funds that healthcare programs have inappropriately disbursed. Thus, key players in the market are investing in the development of solutions compliant with these regulations.
Case Study: Geisinger Health Plan’s Core Administration Transformation Enabling Market Expansion and Margin Improvement
Background
Geisinger Health Plan (GHP), a U.S.-based integrated health plan, operated on a legacy core administration system for over 20 years. As the organization sought to scale and innovate, the outdated system struggled to keep pace with increasing operational complexity and evolving regulatory requirements.
Challenge
The legacy platform resulted in high manual dependency, operational inefficiencies, and limited scalability. It constrained GHP’s ability to introduce new products, expand into new markets, and efficiently manage compliance, ultimately affecting cost margins and overall growth.
Solution
To address these challenges, GHP partnered with Cognizant to implement a modern core administration system leveraging TriZetto Facets, NetworX, and Elements. The solution focused on automating processes, improving system integration, and enabling flexible configuration to enhance efficiency, scalability, and compliance readiness.
Outcome
The transformation delivered significant measurable improvements. Auto-adjudication rates increased from 75% to 85%, reducing manual intervention. Provider payment accuracy reached 99%, and 100% on-time CMS submissions ensured regulatory compliance. In addition, 20 employees were redeployed to higher-value roles, improving productivity and cost efficiency. The new system also enabled faster product launches and supported successful market expansion, strengthening GHP’s competitive position and profitability.
Type Insights
The software segment led the market with the largest revenue share of 56.9% in 2025. The increasing demand for advanced and integrated solutions to streamline administrative processes, reduce operational costs, and enhance efficiency is fueling the growth. In addition, the regulatory changes and compliance requirements necessitate implementing advanced administrative software to ensure accurate and timely claims, billing, and payment processing. Moreover, advancements in technology, including artificial intelligence and machine learning, are enhancing the functionality and effectiveness of these software solutions, making them indispensable tools for healthcare payers.
The services segment is expected to grow at the fastest CAGR over the forecast period. The growth is driven by the increasing complexity of healthcare regulations and policies that require specialized expertise and support for effective compliance and risk management. In addition, the growing adoption of outsourcing models by healthcare payers to manage administrative and IT functions is accelerating demand for specialized service providers. This trend is reinforced by the need to optimize costs, scale, and continuously upgrade systems in a highly regulated environment.
Deployment Insights
The cloud-based segment accounted for the largest market revenue share in 2025 and is anticipated to witness at the fastest CAGR over the forecast period. The growth is driven by the scalability of cloud-based solutions, which allow healthcare payers to efficiently adapt their administrative operations to changing needs. Adopting cloud-based systems also reduces the need for on-premises hardware and maintenance costs, enabling organizations to allocate resources more effectively. Cloud-based solutions offer remote accessibility, enabling collaboration among healthcare professionals regardless of location. This accessibility streamlines patient care and decision-making timelines. Cloud platforms also facilitate the integration of advanced analytics and machine learning algorithms. Rising awareness of the advantages of adopting CAPS is expected to propel market growth over the forecast period.
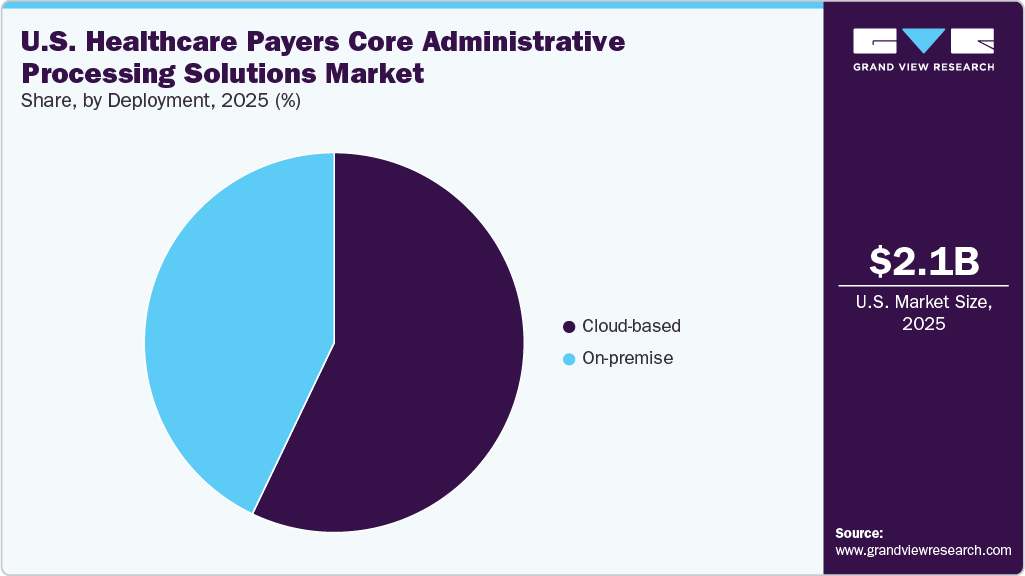
The on-premise segment involves the deployment of core administration processing solutions within the payer’s internal IT infrastructure. This model offers greater control over data security, customization, and compliance management, making it suitable for large payers handling sensitive patient and financial data. However, it requires significant upfront capital investment and ongoing maintenance costs. Despite slower growth than cloud, it remains relevant to organizations with legacy systems and strict regulatory requirements.
Key U.S. Healthcare Payers Core Administrative Processing Solutions Company Insights
Key players are adopting new product development, partnership, and merger & acquisition strategies to increase their market share. Market players such as HealthEdge Software, Inc., Optum, Cognizant, HealthAxis, Plexis Healthcare Systems, Mphasis, and SS&C Technologies dominated the market.
Key U.S. Healthcare Payers Core Administrative Processing Solutions Companies:
- HealthEdge Software, Inc.
- Optum
- Cognizant
- HealthAxis
- Plexis Healthcare Systems
- Mphasis
- SS&C Technologies
- Conduent
- RAM Technologies
- Evolent
- Invidasys
- Advantasure
- VBA software
- Advalent Corp
Recent Developments
-
In September 2025, HealthEdge merged with UST HealthProof to form an AI-powered, end-to-end payer platform, enhancing claims processing, payment integrity, and member engagement capabilities.
-
In March 2024, Cognizant collaborated with Microsoft to leverage generative AI in healthcare management to improve healthcare payers' and On-premise' Typeivity and efficiency. This partnership focuses on the features of the TriZetto Assistant on Facets, leveraging the Azure OpenAI Service and Semantic Kernel to incorporate generative AI capabilities directly into the TriZetto user interface.
-
In October 2022, Optum announced the acquisition of Change Healthcare. This acquisition unites the companies under a shared objective to foster a more streamlined, intelligent, and adaptable health system for patients, payers, and healthcare On-premise. This acquisition aims to streamline core administrative, clinical, and payment processes that are crucial to healthcare on-Premises and payers in delivering patient care. This integration is expected to enhance operational efficiency, reduce complexity, and contribute to overall health system improvements, potentially leading to reduced expenses and improved experiences for all involved parties.
U.S. Healthcare Payers Core Administrative Processing Solutions Market Report Scope
Report Attribute
Details
Market size value in 2026
USD 2.1 billion
Revenue forecast in 2033
USD 3.6 billion
Growth rate
CAGR of 7.5% from 2026 to 2033
Base year for estimation
2025
Historical data
2021 - 2024
Forecast period
2026 - 2033
Quantitative units
Revenue in USD million/billion, and CAGR from 2026 to 2033
Report coverage
Revenue forecast, company ranking, competitive landscape, growth factors, and trends
Segments covered
Type, deployment
Country scope
U.S.
Key companies profiled
HealthEdge Software, Inc.; Optum; Cognizant; HealthAxis; Plexis Healthcare Systems; Mphasis; SS&C Technologies; Conduent; RAM Technologies; Evolent; Invidasys; Advantasure; VBA software; Advalent Corp
Customization scope
Free report customization (equivalent up to 8 analysts working days) with purchase. Addition or alteration to country, regional & segment scope.
Pricing and purchase options
Avail customized purchase options to meet your exact research needs. Explore purchase options
U.S. Healthcare Payers Core Administrative Processing Solutions Market Report Segmentation
This report forecasts revenue growth at the country level and provides an analysis of the latest industry trends in each of the sub-segments from 2021 to 2033. For this study, Grand View Research has segmented the U.S. healthcare payers core administrative processing solutions market report based on type, and deployment.
-
Type Outlook (Revenue, USD Million, 2021 - 2033)
-
Software
-
Standalone
-
Integrated
-
-
Services
-
-
Deployment Outlook (Revenue, USD Million, 2021 - 2033)
-
On-premise
-
Cloud-based
-
Frequently Asked Questions About This Report
b. The U.S healthcare payers core administrative processing solutions market size was estimated at USD 2.0 billion in 2025 and is expected to reach USD 2.1 billion in 2026.
b. The U.S healthcare payers core administrative processing solutions market is expected to grow at a compound annual growth rate of 7.5% from 2026 to 2033 to reach USD 3.6 billion by 2033.
b. Software dominated the U.S healthcare payers core administrative processing solutions market with a share of 56.9% in 2025. This is attributable to the increasing demand for advanced and integrated solutions to streamline administrative processes, reduce operational costs, and enhance efficiency.
b. Some key players operating in the U.S healthcare payers core administrative processing solutions market include HealthEdge Software, Inc.; Optum; Cognizant; HealthAxis; Plexis Healthcare Systems; Mphasis; SS&C Technologies; Conduent; RAM Technologies; Evolent; Invidasys; Advantasure; VBA software; Advalent Corp
b. Key factors driving market growth include the growing demand for cost reduction, technological advancements, the modernization of enrollment and billing processes, the increasing adoption of strategic initiatives by market players, and evolving regulatory and compliance requirements.
Share this report with your colleague or friend.
Need a Tailored Report?
Customize this report to your needs — add regions, segments, or data points, with 20% free customization.

ISO 9001:2015 & 27001:2022 Certified
We are GDPR and CCPA compliant! Your transaction & personal information is safe and secure. For more details, please read our privacy policy.
Trusted market insights - try a free sample
See how our reports are structured and why industry leaders rely on Grand View Research. Get a free sample or ask us to tailor this report to your needs.