- Home
- »
- Healthcare IT
- »
-
Artificial Intelligence For Healthcare Payer Market Report, 2033GVR Report cover
![Artificial Intelligence For Healthcare Payer Market Size, Share & Trends Report]()
Artificial Intelligence For Healthcare Payer Market (2025 - 2033) Size, Share & Trends Analysis Report By Component (Software, Services), By Deployment, By Application, By Technology, By Region, And Segment Forecasts
- Report ID: GVR-4-68040-315-1
- Number of Report Pages: 120
- Format: PDF
- Historical Range: 2021 - 2023
- Forecast Period: 2025 - 2033
- Industry: Healthcare
- Report Summary
- Table of Contents
- Segmentation
- Methodology
- Download FREE Sample
-
Download Sample Report
Artificial Intelligence For Healthcare Payer Market Summary
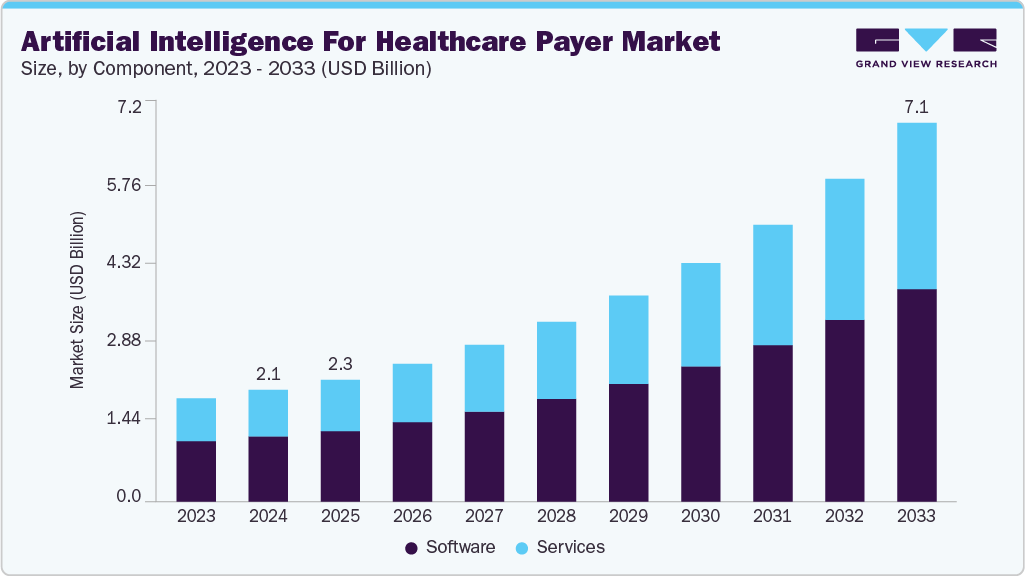
The global artificial intelligence for healthcare payer market size was estimated at USD 2.11 billion in 2024 and is projected to reach USD 7.15 billion by 2033, growing at a CAGR of 15.26% from 2025 to 2033. The rising demand for efficient and cost-effective healthcare solutions has accelerated the adoption of AI technologies.
Key Market Trends & Insights
- North America dominated the artificial intelligence (AI) for healthcare payer market with the largest revenue share of 37.45% in 2024.
- The artificial intelligence (AI) for healthcare payer market in the U.S. accounted for the largest market revenue share in North America in 2024.
- Based on the component, the software segment led the market with the largest revenue share of 57.89% in 2024.
- Based on deployment, the cloud segment led the market with the largest revenue share of 58.01% in 2024.
- Based on application, the claims processing optimization segment held the largest market share of 37.77% in 2024.
Market Size & Forecast
- 2024 Market Size: USD 2.11 Billion
- 2033 Projected Market Size: USD 7.15 Billion
- CAGR (2025-2033): 15.26%
- North America: Largest market in 2024
Artificial intelligence helps in automating administrative tasks, reducing operational costs, and enhancing the accuracy of claims processing, thereby improving overall efficiency. In addition, the growing volume of healthcare data necessitates advanced analytics, which AI can provide, offering deeper insights into patient care and outcomes. Moreover, regulatory changes and the increasing focus on value-based care models push payers to adopt artificial intelligence to improve patient engagement and satisfaction while managing risks more effectively.Advancements in machine learning and natural language processing enable artificial intelligence systems to understand better and analyze complex medical data, leading to more informed decision-making. The continuous innovation in artificial intelligence technologies, along with the strategic partnerships between AI companies and healthcare payers, also plays a crucial role in market expansion. For instance, in April 2024, Pager, Inc., announced the development of three new applications utilizing Google Cloud's advanced generative AI (GenAI) capabilities. These GenAI applications aim to support the fourfold aim of care by alleviating the administrative burden on multidisciplinary care teams and fostering a more personalized and conversational experience for members. This enhanced interaction aids members in navigating, coordinating, and taking the next best steps in their healthcare journey.
Furthermore, fraudulent activities in healthcare claims are a significant concern for payers, leading to substantial financial losses. Artificial intelligence and machine learning algorithms excel in detecting anomalous patterns indicative of fraud. These technologies analyze historical claims data to identify suspicious activities in real time, allowing for prompt investigation and mitigation. By reducing fraud, healthcare payers are able to safeguard their financial resources and ensure that funds are appropriately allocated to genuine claims, thereby maintaining the integrity of the healthcare system.
The shift from fee-for-service to value-based care models places a greater emphasis on patient outcomes and cost efficiency. Artificial intelligence plays a pivotal role in this transition by enabling healthcare payers to analyze patient data and measure the effectiveness of care interventions. Predictive analytics help identify patients who would benefit most from preventive care and early interventions, thereby reducing hospital readmissions and improving long-term health outcomes. By supporting value-based care initiatives, artificial intelligence helps payers align with industry trends and deliver better value to members. For instance, in January 2025, Innovaccer acquired Humbi AI, an actuarial software and analytics firm, to enhance its Healthcare Intelligence Cloud with advanced actuarial capabilities. This move brought significant benefits, including enhanced contract performance, improved payer benchmarking, and optimized provider network management. These factors collectively contribute to the rapid growth of artificial intelligence in the healthcare payer market, promising improved efficiency, reduced costs, and enhanced patient care.
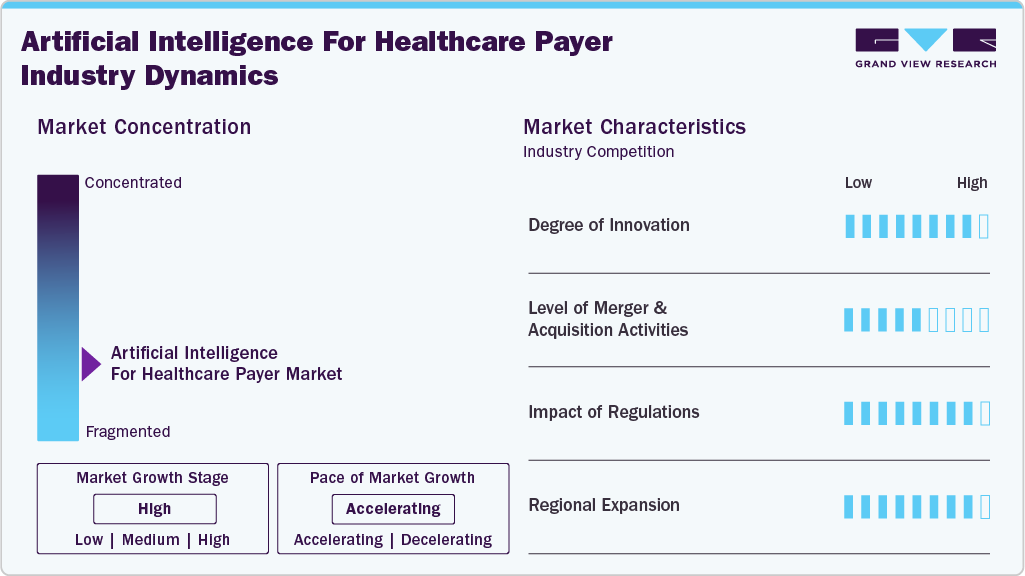
Market Concentration & Characteristics
The chart below illustrates the relationship between market concentration, market characteristics, and market participants. The x-axis represents the level of market concentration, ranging from low to high. The y-axis represents various market characteristics, including industry competition, degree of innovation, level of M&A activities, impact of regulations, and regional expansion. Market growth is high, and the pace of the market growth is accelerating. For instance, the AI for healthcare payers market is highly fragmented, with many small players entering the market and launching new innovative products. The degree of innovation, the impact of regulations on the industry, and the regional expansion of the market is high. The level of M&A activities in the market appears to be moderate.
The degree of innovation in artificial intelligence (AI) for healthcare payer industry is substantial. It continues to evolve rapidly, driven by advancements in technology and increasing demands for efficiency and personalization in healthcare services. For instance, in June 2025, SAS launched SAS Health Cost of Care Analytics, an AI-powered solution for healthcare payers and providers to analyze claims as episodes of care using clinical definitions. The platform includes risk-based provider performance comparisons and supports simplified data management.
Key players are implementing strategic initiatives, such as collaborations, geographical expansion, and partnerships, to strengthen their market presence. For instance, in February 2024, Veradigm LLC acquired ScienceIO. Veradigm to utilize ScienceIO’s advanced Healthcare Artificial Intelligence Platform with its extensive, high-quality data set to develop private language models for healthcare. The acquisition is expected to expedite platform enhancements across the Veradigm network, benefiting provider, payer, and life sciences sectors.
Regulations on artificial intelligence (AI) for healthcare payer industry have intensified, focusing on data privacy, security, and ethical standards. Recent trends include stricter compliance requirements, transparency in AI decision-making, and enhanced guidelines to ensure patient safety and equitable access, driving more robust and trustworthy AI implementations in healthcare.
As the healthcare sector moves towards a value-based care approach, integrating data into claims adjudication within this ecosystem becomes increasingly crucial. Through the utilization of AI-based data analytics and emerging technologies, healthcare payers can mitigate errors, alleviate operational challenges, and ultimately enhance efficiency. This enables them to align incentives with patient outcomes better, foster improved care coordination, and nurture a healthcare system centered around patients.
Component Insights
The software segment led the market with the largest revenue share of 57.89% in 2024. This is attributed to the increasing demand for advanced analytics capabilities to harness the vast amount of healthcare data that drives the adoption of AI-powered software solutions. These solutions offer predictive analytics, machine learning algorithms, and natural language processing capabilities, enabling payers to extract actionable insights and improve decision-making processes. Moreover, the need for automation and efficiency in administrative tasks, such as claims processing and member enrollment, fuels the demand for AI-driven software solutions.
The services segment is expected to grow at the fastest CAGR over the forecast period. These services include consulting, integration, training, and ongoing support that ensure smooth deployment of AI solutions across payer workflows such as claims processing, fraud detection, and risk adjustment. Service providers guide organizations in tailoring AI platforms to align with compliance requirements and organizational objectives. By offering expertise in regulatory frameworks and data governance, they help payers mitigate risks associated with sensitive patient information.
Deployment Insights
The cloud segment led the market with the largest revenue share of 58.01% in 2024. In addition, this segment is anticipated to grow at the fastest CAGR during the forecast period. The scalability and flexibility of cloud infrastructure enable healthcare payers to efficiently deploy and manage artificial intelligence applications, accommodating fluctuating workloads and expanding data volumes.
Cloud platforms offer advanced AI services, such as machine learning algorithms and natural language processing tools, allowing payers to harness powerful capabilities without significant upfront investments in hardware or software development. Moreover, enhanced data security and compliance measures provided by reputable cloud providers address concerns regarding patient privacy and regulatory requirements, further driving the adoption of cloud-based solutions.
Application Insights
Based on application, the claims processing optimization segment held the largest market share of 37.77% in 2024. Efficient claim processing is vital for ensuring timely reimbursement, cost reduction, fraud prevention, and fostering positive provider relationships. With a growing population of insured individuals and increasing demand for healthcare services, the volume of insurance claims is also on the rise. Therefore, optimizing claim processing becomes imperative to meet these demands effectively while maintaining accuracy and efficiency. Moreover, regulatory requirements and compliance standards compel payers to invest in AI-powered solutions for claims processing to ensure adherence to industry regulations and standards.
According to an article published by Mastek in March 2024, an analysis of health insurance claims administered by a mid-sized payer with 1.5 million members highlighted that 70% of claims were identified as anomalous, necessitating manual review. Using machine learning with past claim data allows for a flexible response system, surpassing static rules that may not fully assess each case.
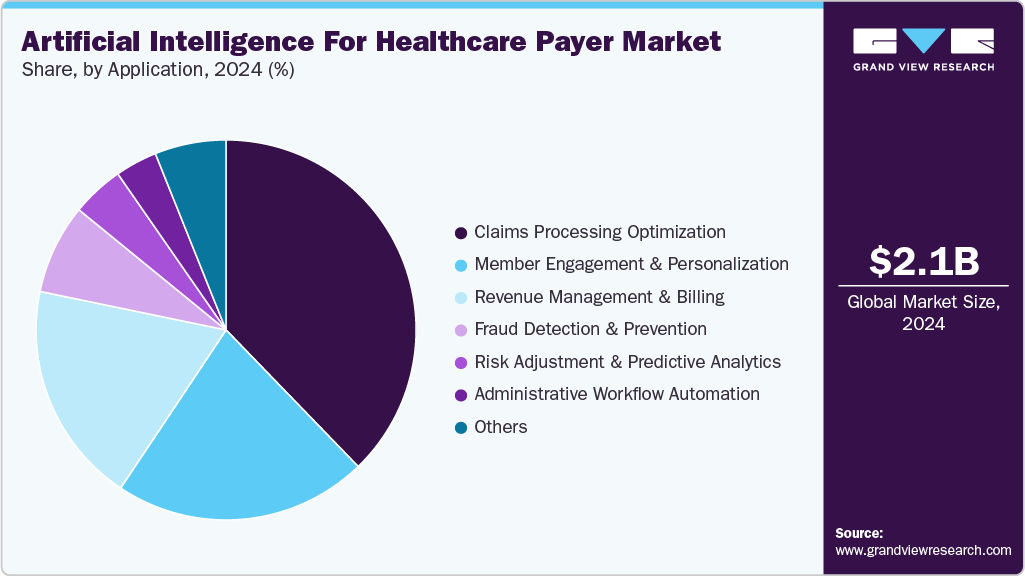
The revenue management and billing segment is expected to grow at the fastest CAGR over the forecast period. The increasing complexity of healthcare billing regulations and payer-provider contracts necessitates sophisticated solutions to ensure compliance and streamline revenue workflows. Artificial intelligence applications in revenue management and billing address these challenges by automating coding, documentation, and claims submission processes, reducing administrative burdens, and enhancing overall operational efficiency. AI technologies offer advanced analytics capabilities that enable more accurate and efficient revenue cycle management. Such factors would likely fuel the segment growth.
Regional Insights
North America dominated the artificial intelligence (AI) for healthcare payer market with the largest revenue share of 37.45% in 2024. The regional growth is propelled by factors such as increasing adoption of AI technologies to automate claims processing, detect fraud and abuse, and optimize network management. Moreover, the adoption of AI-powered virtual assistants and chatbots is enhancing customer service and engagement, providing members with personalized support and guidance. As the demand for efficient and cost-effective healthcare solutions continues to rise, artificial intelligence is poised to play an increasingly vital role in shaping the future of the healthcare payer market in North America.
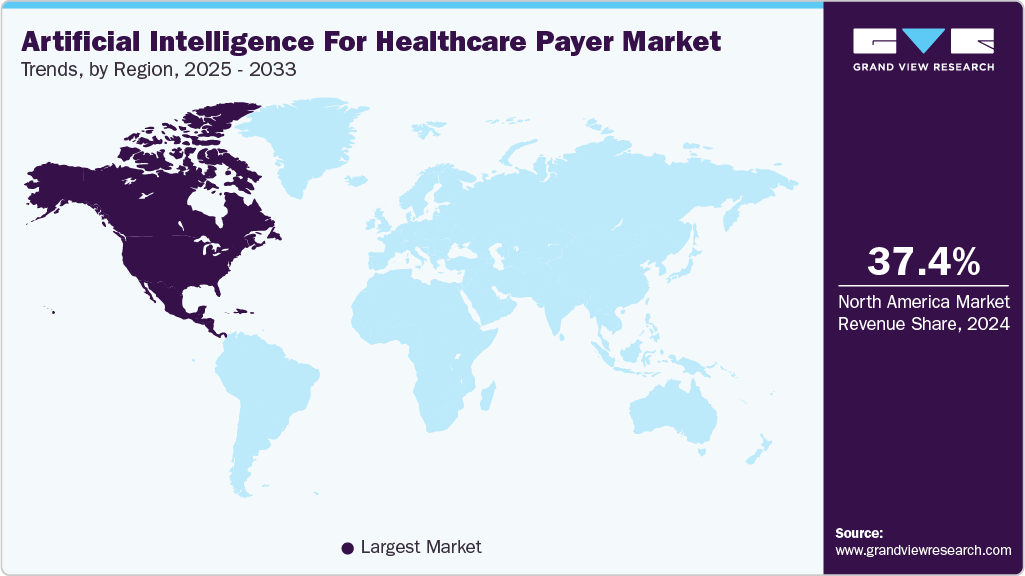
U.S. Artificial Intelligence (AI) for Healthcare Payer Market Trends
The artificial intelligence (AI) for healthcare payer market in the U.S. accounted for the largest market revenue share in North America in 2024. This is attributed to the increasing convergence of technological advancements, regulatory support, and the imperative for improved healthcare outcomes fuel the growth of AI within the healthcare payer market in the U.S.
Europe Artificial Intelligence (AI) for Healthcare Payer Market Trends
The artificial intelligence (AI) for healthcare payer market in Europe is driven by strong policy support for digital health transformation. The European Commission’s funding initiatives, such as Horizon Europe and the EU4Health program, accelerate AI adoption for insurance risk assessment and fraud detection.
The UK artificial intelligence (AI) for healthcare payer market held the largest market share in the European region in 2024. This growth is fueled by the government’s emphasis on innovation within the National Health Service (NHS). The NHS Long Term Plan highlights digitalization and AI integration for efficient claims management and fraud prevention. Health insurers are increasingly leveraging AI to personalize member engagement and improve claims turnaround times.
The Germany artificial intelligence (AI) for healthcare payer market is driven by the country’s Digital Healthcare Act, which promotes reimbursement for digital health solutions. The country’s high healthcare expenditure creates a strong incentive for predictive analytics to optimize risk adjustment. AI is also being utilized to improve member engagement in both public and private insurance sectors.
Asia Pacific Artificial Intelligence (AI) for Healthcare Payer Market Trends
The artificial intelligence (AI) for healthcare payer market in Asia Pacific is anticipated to witness at a significant CAGR over the forecast years. The increasing cost of healthcare services in the region has led payers to seek innovative solutions to manage expenses while maintaining quality. Artificial intelligence offers avenues for cost reduction through predictive analytics, fraud detection, and claims processing automation. For instance, in June 2025, India-based Star Health Insurance partnered with Medi Assist in June 2025 to adopt the AI-driven MAtrix platform to modernize claims processing. The platform aims to accelerate claim settlements, enhance accuracy, reduce manual processes, and detect fraud more effectively through advanced AI and machine learning.
TheChina artificial intelligence (AI) for healthcare payer market is anticipated to grow at the fastest CAGR during the forecast period. Healthcare payers in China are under pressure to improve operational efficiency and provide better services to their members. AI-driven solutions such as claims processing automation, virtual assistants for customer support, and predictive analytics for risk assessment are increasingly being adopted to meet these demands. Moreover, the China government has been actively promoting the adoption of artificial intelligence in healthcare to improve efficiency, reduce costs, and enhance patient care. Initiatives like the "Healthy China 2030" plan emphasize the importance of technology, including AI, in transforming the healthcare sector.
Latin America Artificial Intelligence (AI) for Healthcare Payer Market Trends
The artificial intelligence (AI) for healthcare payer market in Latin America is expected to grow at a significant CAGR over the forecast period. Latin American countries have been steadily increasing their healthcare expenditure to improve healthcare services and infrastructure. This increased investment has paved the way for the adoption of advanced technologies like AI in healthcare.
MEA Artificial Intelligence (AI) for Healthcare Payer Market Trends
The artificial intelligence (AI) for healthcare payer market in the MEA is expected to grow at a significant CAGR over the coming years. There is a growing awareness and acceptance of artificial intelligence technologies within the healthcare industry in the MEA region. Payers are recognizing the potential benefits of artificial intelligence in terms of cost savings, operational efficiency, and improved patient outcomes, driving investment in AI solutions.
Key Artificial Intelligence for Healthcare Payer Company Insights
Key players are adopting various strategies such as product development, partnerships, funding, and investments, driving the artificial intelligence (AI) for healthcare payer industry. The willingness of healthcare payers to adopt artificial intelligence technologies impacts market share, with early adopters gaining competitive advantages. Startups are also significantly contributing to the innovation ecosystem, with companies like Lyric.ai, Softheon, ZS, and more providing niche AI solutions aimed at optimizing operational efficiencies and improving patient care pathways.
Key Artificial Intelligence for Healthcare Payer Companies
The following are the leading companies in the artificial intelligence (AI) for healthcare payer market. These companies collectively hold the largest market share and dictate industry trends.
- Nuance Communications (Microsoft)
- AiRo Digital Labs
- Accenture
- Cognizant
- CareCloud, Inc.
- MST Solutions, L.L.C.
- Hexaware Technologies Limited
- Innovaccer, Inc.
- Oracle
- Codoxo
- Amelia US LLC
- R1 RCM Inc
Recent Developments
-
In September 2025, Milliman MedInsight launched the Innovation Portal, an AI-powered, cloud-based analytics platform for healthcare organizations, including payers.
-
In August 2025, Firstsource Solutions and Guidehealth formed a strategic partnership to accelerate AI-enabled value-based care innovation for health plans. The collaboration combines Firstsource’s AI-first technology and UnBPO transformation model with Guidehealth’s expertise in value-based care innovation.
-
In March 2025, TrampolineAI, an AI-powered contact center platform for health plans, was launched out of Redesign Health, a healthcare innovation company. The product integrates with existing phone systems to deliver agents real-time member information, step-by-step call guidance, automated call summaries, and real-time sentiment and compliance monitoring.
-
In February 2025, AArete launched Doczy.ai, an AI-powered healthcare payer solution that digitizes and analyzes complex provider contracts to improve operational efficiency. It enhances payment accuracy, reduces administrative costs, ensures compliance, and provides actionable insights by interpreting contract language using large language models.
-
In November 2024, HealthEdge and Codoxo announced a strategic partnership to transform payment integrity for healthcare payers using generative AI (GenAI). Integrating HealthEdge Source, an advanced payment integrity solution, with Codoxo’s GenAI-driven Unified Cost Containment Platform, the collaboration streamlines payment workflows, reduces vendor complexity, improves payment accuracy, enhances fraud detection, and accelerates time-to-value.
-
In November 2024, Tassat Group partnered with Veuu to use AI and blockchain technology to enhance transparency in healthcare claims and payment processes.
-
In March 2024, Microsoft and Cognizant entered into a collaboration agreement to integrate generative AI into healthcare. The goal behind the strategy is to enhance productivity and efficiency for healthcare providers and payers, while prioritizing timely responses and elevating patient care. Through the utilization of Azure OpenAI Service and Semantic Kernel, the TriZetto Assistant on Facets will incorporate generative AI directly into the TriZetto user interface, facilitating seamless access to advanced AI capabilities.
-
In July 2023, Codoxo launched its latest solution, ClaimPilot for healthcare payers. This cutting-edge generative AI offering is designed to enhance the efficiency of healthcare cost containment and payment integrity programs significantly.
"Generative AI has the potential to inject USD 1 trillion into the U.S. economy over the next decade through new revenue streams, operational efficiency, and innovation in products, services and ways of working "
- said Surya Gummadi, EVP and President, Cognizant Americas.
Artificial Intelligence for Healthcare Payer Market Report Scope
Report Attribute
Details
Market size value in 2025
USD 2.29 billion
Revenue forecast in 2033
USD 7.15 billion
Growth rate
CAGR of 15.26% from 2025 to 2033
Base year for estimation
2024
Historical data
2021 - 2023
Forecast period
2025 - 2033
Quantitative units
Revenue in USD million/billion and CAGR from 2025 to 2033
Report coverage
Revenue forecast, company ranking, competitive landscape, growth factors, and trends
Segments covered
Component, deployment, technology, application, region
Regional scope
North America; Europe; Asia Pacific; Latin America; MEA
Country scope
U.S.; Canada; Mexico; Germany; UK; France; Italy; Spain; Sweden; Denmark; Norway; China; Japan; India; South Korea; Australia; Thailand; Brazil; Argentina; UAE; South Africa; Saudi Arabia; and Kuwait
Key companies profiled
Nuance Communications (Microsoft); AiRo Digital Labs; Accenture; Cognizant; CareCloud, Inc.; MST Solutions; L.L.C.; Hexaware Technologies Limited; Innovaccer, Inc.; Oracle; Codoxo; Amelia US LLC; R1 RCM Inc.
Customization scope
Free report customization (equivalent up to 8 analysts working days) with purchase. Addition or alteration to country, regional & segment scope.
Pricing and purchase options
Avail customized purchase options to meet your exact research needs. Explore purchase options
Global Artificial Intelligence (AI) for Healthcare Payer Market Report Segmentation
This report forecasts revenue growth at global, regional, and country levels and provides an analysis of the latest industry trends in each of the sub-segments from 2021 to 2033. For this study, Grand View Research has segmented the global artificial intelligence (AI) for healthcare payer market report based on the component, deployment, technology, application, and region.
-
Component Outlook (Revenue, USD Million, 2021 - 2033)
-
Software
-
Services
-
-
Deployment Outlook (Revenue, USD Million, 2021 - 2033)
-
Cloud
-
On-Premises
-
-
Technology Outlook (Revenue, USD Million, 2021 - 2033)
-
Machine Learning (ML)
-
Natural Language Processing (NLP)
-
Robotic Process Automation (RPA)
-
Predictive Analytics
-
Generative AI
-
-
Application Outlook (Revenue, USD Million, 2021 - 2033)
-
Claims Processing Optimization
-
Fraud Detection and Prevention
-
Revenue Management and Billing
-
Member Engagement and Personalization
-
Risk Adjustment & Predictive Analytics
-
Administrative Workflow Automation
-
Others
-
-
Regional Outlook (Revenue, USD Million, 2021 - 2033)
-
North America
-
U.S.
-
Canada
-
Mexico
-
-
Europe
-
UK
-
Germany
-
France
-
Italy
-
Spain
-
Norway
-
Sweden
-
Denmark
-
-
Asia Pacific
-
Japan
-
China
-
India
-
Thailand
-
Australia
-
South Korea
-
-
Latin America
-
Brazil
-
Argentina
-
-
Middle East and Africa
-
Saudi Arabia
-
South Africa
-
UAE
-
Kuwait
-
-
Share this report with your colleague or friend.
Need a Tailored Report?
Customize this report to your needs — add regions, segments, or data points, with 20% free customization.

ISO 9001:2015 & 27001:2022 Certified
We are GDPR and CCPA compliant! Your transaction & personal information is safe and secure. For more details, please read our privacy policy.
Trusted market insights - try a free sample
See how our reports are structured and why industry leaders rely on Grand View Research. Get a free sample or ask us to tailor this report to your needs.