- Home
- »
- Healthcare IT
- »
-
U.S. Healthcare Data Monetization Market Size Report, 2033GVR Report cover
![U.S. Healthcare Data Monetization Market For Quality, Outcomes & Payment Intelligence Size, Share & Trends Report]()
U.S. Healthcare Data Monetization Market (2026 - 2033) For Quality, Outcomes & Payment Intelligence Size, Share & Trends Analysis Report By Entity (Healthcare Entities, Non-healthcare Entities), By Product Type (Data Subscription), By Buyer, By Buyer Vs Product Type, And Segment Forecasts
- Report ID: GVR-4-68040-907-7
- Number of Report Pages: 90
- Format: PDF
- Historical Range: 2021 - 2025
- Forecast Period: 2026 - 2033
- Industry: Healthcare
- Report Summary
- Table of Contents
- Segmentation
- Methodology
- Download FREE Sample
-
Download Sample Report
U.S. Healthcare Data Monetization Market For Quality, Outcomes & Payment Intelligence Summary
The U.S. healthcare data monetization market size for quality, outcomes & payment intelligence (serviceable obtainable market) was estimated at USD 955.44 million in 2025 and is projected to reach USD 1,705.53 million by 2033, growing at a CAGR of 7.77% from 2026 to 2033. This growth is driven by the rapid expansion of healthcare data volume (EHR, Claims, Wearables), rising demand for Real-World Data (RWD) & Real-World Evidence (RWE), increasing adoption of AI, advanced analytics & cloud platforms, and growing payer focus on cost optimization & risk management.
Key Market Trends & Insights
- Based on entity, the healthcare entities segment led the market with the largest revenue share of 94.8% in 2025.
- Based on product type, the pharmaceutical companies segment led the market with the largest revenue share in 2025.
- The insights-as-a-service (curated analytics products) segment accounted for the leading revenue share of 40.10% in 2025.
Market Size & Forecast
- 2025 Market Size: USD 955.44 Million
- 2033 Projected Market Size: USD 1,705.53 Million
- CAGR (2026-2033): 7.77%
The U.S. healthcare ecosystem generates massive datasets through widespread adoption of electronic health records (EHRs), imaging systems, claims databases, and connected devices. This exponential growth in structured and unstructured data creates a large monetizable asset base, enabling providers and payers to commercialize de-identified datasets and insights.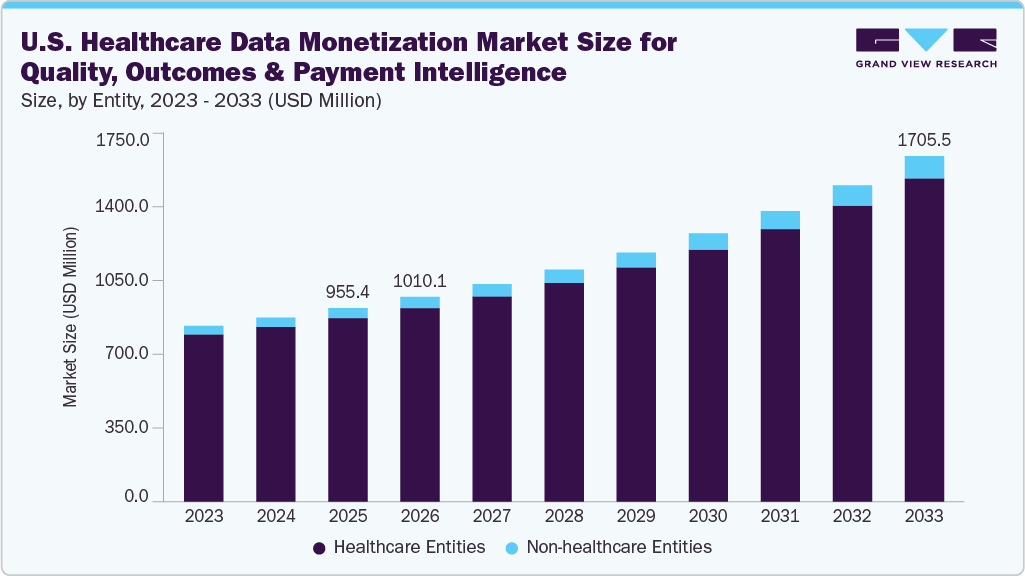
Moreover, there is a significant shift in the U.S. life sciences ecosystem toward leveraging real-world data (RWD) and generating real-world evidence (RWE) to complement traditional clinical trial data. Pharmaceutical and biotechnology companies are increasingly utilizing these datasets to optimize clinical trial design, identify eligible patient populations, monitor treatment outcomes, and support regulatory submissions.
In addition, regulators and payers are placing greater emphasis on post-market evidence to assess drug efficacy and cost-effectiveness in real-world settings. This growing reliance on RWD/RWE has created a strong demand for high-quality, longitudinal patient datasets, encouraging healthcare providers and data aggregators to monetize their data assets through partnerships, licensing agreements, and analytics services. As a result, data monetization is becoming deeply embedded in the broader drug development and commercialization lifecycle.
Market Concentration & Characteristics
The degree of innovation in the U.S. healthcare data monetization market for quality, outcomes & payment intelligence is low. Organizations are leveraging real-world data, predictive modeling, and cloud-based platforms to link clinical quality with financial outcomes and reimbursement optimization. The shift toward value-based care is accelerating innovation in outcomes-based analytics and risk-sharing models, enabling payers and providers to monetize insights while improving care quality and cost efficiency.
The level of M&A activity in the U.S. healthcare data monetization industry for quality, outcomes & payment intelligence is increasing, as companies work with healthcare providers, digital health platforms, and research organizations to expand access to nutrition-based healthcare solutions and improve patient outcomes.
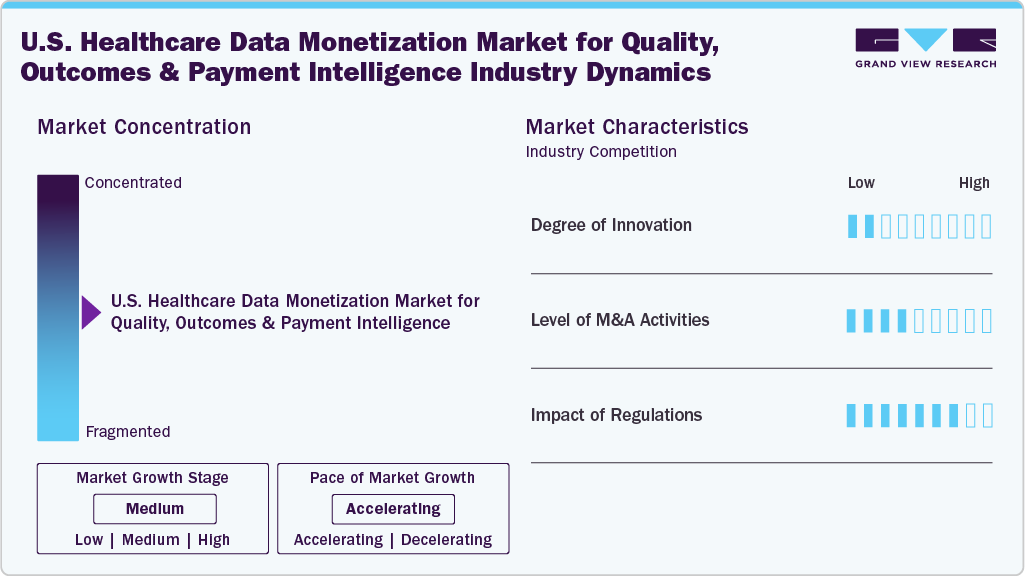
Regulation plays a dual role, both enabling and constraining the U.S. healthcare data monetization market for quality, outcomes, and payment intelligence. On one hand, frameworks such as HIPAA and interoperability mandates (e.g., TEFCA under the 21st Century Cures Act) create structured, secure data exchange environments, enabling the use of real-world data for outcomes measurement, value-based reimbursement, and payment intelligence. These regulations support standardized data sharing and accelerate analytics adoption across payers and providers. On the other hand, stringent privacy laws impose high compliance costs, data anonymization requirements, and legal risks, limiting the free commercialization of patient-level data. Concerns around re-identification, penalties, and evolving regulatory ambiguity often slow innovation and restrict participation, particularly in outcomes-linked monetization models.
Entity Insights
The healthcare entities segment accounted for the largest revenue share of the U.S. healthcare data monetization industry for quality, outcomes & payment intelligence in 2025.Healthcare entities are the core drivers of the healthcare data monetization ecosystem, as they both generate and actively utilize clinical, operational, and patient-level data. This segment includes pharmaceutical companies, health systems & providers, retail pharmacies, and other healthcare-focused organizations. Growth in this segment is driven by the continued shift toward value-based care models, rising regulatory and reporting requirements, the increasing complexity of patient journeys, and the need for real-world evidence in both clinical and commercial settings. In addition, growing digitalization across healthcare systems and the expansion of integrated care networks are further accelerating data adoption.
The non-healthcare segment is expected to grow at the fastest CAGR over the forecast period. The growth of this segment is driven by increasing interest in healthcare as an investment and innovation domain, rising employer focus on healthcare cost management, expanding role of data in strategic decision-making, and the entry of technology players leveraging AI and advanced analytics. The growing availability of structured healthcare datasets is further enabling broader participation from non-traditional buyers.
Healthcare Entities Market, by Product Type Insights
The insights-as-a-service (curated analytics products) segment accounted for the leading revenue share of 40.10% in 2025. Insights-as-a-service is a monetization model in which healthcare organizations deliver actionable, pre-analyzed insights derived from integrating multiple data sources using advanced analytics methodologies. This approach focuses on delivering decision-ready outputs, enabling end users to use insights without extensive data processing or analytical effort. The adoption of insights-as-a-service offerings is driven by the increasing preference for pre-processed, analytics-ready outputs, particularly among organizations with limited in-house data integration and analytics capabilities. These solutions reduce the complexity of data ingestion, standardization, and model development, enabling faster, more efficient decision-making.
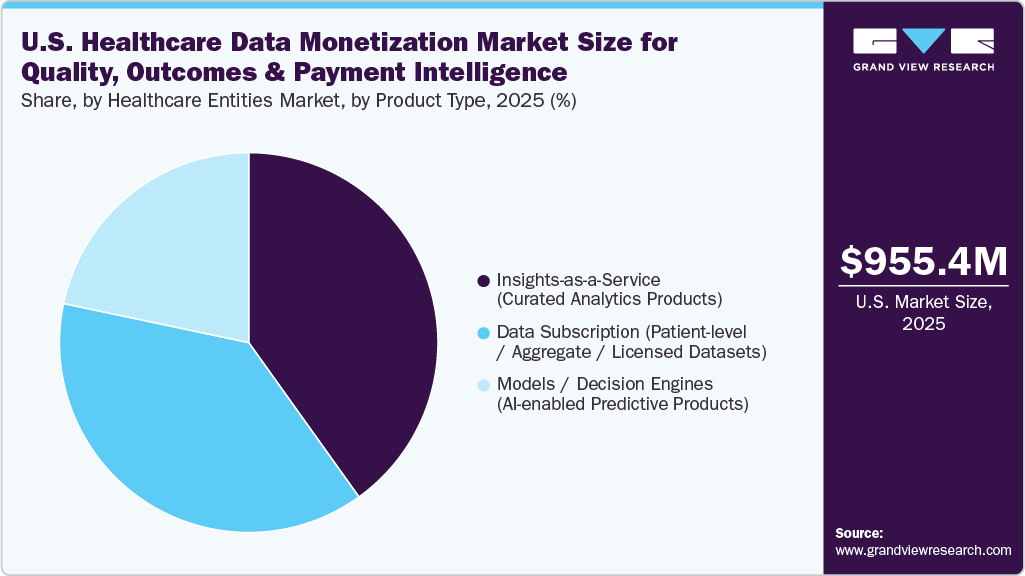
The models / decision engines (AI-enabled predictive products) segment is expected to grow significantly over the forecast period. Models and decision engines represent an advanced product type in the U.S. healthcare data monetization market, in which organizations commercialize algorithm-driven outputs that generate predictions, recommendations, or automated decisions based on underlying healthcare data. These products are typically built using trained machine learning (ML), artificial intelligence (AI), or statistical models and are deployed to support real-time or near-real-time decision-making across clinical, operational, and financial use cases.
These solutions operate by ingesting multi-source datasets, including claims, electronic health records (EHRs), laboratory results, and behavioral or utilization data, and applying trained models to identify patterns, forecast outcomes, and trigger decision pathways. Outputs are often embedded directly into clinical systems, payer platforms, or workflow tools, enabling functionalities such as risk scoring, readmission prediction, disease progression modeling, fraud detection, and reimbursement optimization.
Key U.S. Healthcare Data Monetization for Quality, Outcomes & Payment Intelligence Company Insights
The competitive landscape is highly fragmented yet innovation-driven, with large tech firms providing infrastructure. At the same time, specialized healthcare analytics companies drive value creation in quality measurement, outcomes tracking, and payment optimization models.
Key U.S. Healthcare Data Monetization for Quality, Outcomes & Payment Intelligence Companies:
- Optum, Inc.
- Komodo Health, Inc.
- Cotiviti, Inc.
- IQVIA
- Inovalon
- Symphony Health
- Definitive Healthcare
- Truveta
- Arcadia Solutions, LLC
U.S. Healthcare Data Monetization Market for Quality, Outcomes & Payment Intelligence Report Scope
Report Attribute
Details
Market SOM size value in 2026
USD 1,010.13 million
Market TAM size value in 2026
USD 8,171.23 million
SOM Revenue forecast in 2033
USD 1,705.53 million
TAM Revenue forecast in 2033
USD 12,099.50 million
Growth Rate (SOM market)
CAGR of 7.77% from 2026 to 2033
Actual data
2021 - 2025
Forecast period
2026 - 2033
Quantitative units
Revenue in USD million and CAGR from 2026 to 2033
Report coverage
Revenue forecast, company ranking, competitive landscape, growth factors, and trends
Segments covered
Entity, product type, buyer, buyer vs product type
Key companies profiled
Optum, Inc.; Komodo Health, Inc.; Cotiviti, Inc.; IQVIA; Inovalon; Symphony Health; Definitive Healthcare; Truveta; Arcadia Solutions, LLC
Customization scope
Free report customization (equivalent up to 8 analysts working days) with purchase. Addition or alteration to country, regional & segment scope.
Pricing and purchase options
Avail customized purchase options to meet your exact research needs. Explore purchase options
U.S. Healthcare Data Monetization Market Report Segmentation
This report forecasts revenue growth analysis of the latest industry trends in each of the sub-segments from 2021 to 2033. For this study, Grand View Research has segmented the U.S. healthcare data monetization market for quality, outcomes & payment intelligence report based on entity, product type, buyer type, and buyer vs product sub-segmentation:
-
Entity Outlook (TAM, SAM & SOM, USD Million, 2021 - 2033)
-
Healthcare entities
-
Non-healthcare entities
-
-
Healthcare Entities Outlook (SAM & SOM, USD Million, 2021 - 2033)
-
By Product Type
-
Data Subscription (patient-level / aggregate / licensed datasets)
-
Insights-as-a-Service (curated analytics products)
-
Models / Decision Engines (AI-enabled predictive products)
-
-
By Buyer Type
-
Pharmaceutical Companies
-
Clinical Trial Enablement (Site selection, patient identification, feasibility analytics)
-
HCP & Customer Targeting (Physician targeting, segmentation, sales enablement)
-
Safety, Adherence & HEOR (RWE, adherence analytics, pharmacovigilance, outcomes tracking)
-
Formulary Analytics / Commercial Access Enablement (Market access, payer strategy, reimbursement analytics)
-
-
Health Systems & Providers
-
Go-to-Market & Contracting (Value-based care enablement, service line optimization)
-
Quality & Care Gap Closure (HEDIS, Stars, performance improvement)
-
Network & Operational Optimization (Referral management, capacity optimization, leakage reduction)
-
Formulary Analytics / Commercial Access Enablement (Market access, payer strategy, reimbursement analytics)
-
-
Retail Pharmacies
-
Independent Pharmacies
-
Chain Pharmacies
-
-
Other Non-Payer Healthcare Entities
-
-
-
Buyer vs Product Type Sub-Segmentation Outlook (SAM & SOM, USD Million, 2021 - 2033)
-
Pharmaceutical Companies
-
Clinical Trial Enablement (Site selection, patient identification, feasibility analytics)
-
Data subscription (clinical + claims + quality datasets)
-
Insights service (trial feasibility analytics)
-
Model/engines (site selection AI tools)
-
-
HCP & Customer Targeting (Physician targeting, segmentation, sales enablement)
-
Data (HCP-level claims + quality signals)
-
Insights (targeting analytics)
-
Models (real-time targeting engines)
-
-
Safety, Adherence & HEOR (RWE, adherence analytics, pharmacovigilance, outcomes tracking)
-
Data (payer + quality + reimbursement datasets)
-
Insights (access analytics)
-
Models (pricing / access optimization tools)
-
-
Formulary Analytics / Commercial Access Enablement (Market access, payer strategy, reimbursement analytics)
-
Data (payer + quality + reimbursement datasets)
-
Insights (access analytics)
-
Models (pricing / access optimization tools))
-
-
-
Health Systems & Providers
-
Data (EMR + claims + quality data)
-
Insights (care gap + operational analytics)
-
Models (VBC optimization engines))
-
-
Retail Pharmacies
-
Data (patient + prescription + adherence signals)
-
Insights (patient behavior / refill optimization)
-
Models (adherence / engagement engines)
-
-
Other Non-Payer Healthcare Entities
-
Data packages
-
Insights platforms
-
API / embedded models
-
-
Frequently Asked Questions About This Report
b. The U.S. healthcare data monetization market size for quality, outcomes & payment intelligence (Serviceable Obtainable Market) was estimated at USD 955.44 million in 2025 and is expected to reach USD 1,010.13 million in 2026.
b. The U.S. healthcare data monetization market size for quality, outcomes & payment intelligence is expected to grow at a compound annual growth rate of 7.77% from 2026 to 2033 to reach USD 1,705.53 million by 2033.
b. Based on entities the healthcare entities segment accounted for the largest revenue share in 2025. Healthcare entities are the core drivers of the healthcare data monetization ecosystem, as they both generate and actively utilize clinical, operational, and patient-level data.
b. Some key players operating in the U.S. healthcare data monetization market size for quality, outcomes & payment intelligence include Optum, Inc., Komodo Health, Inc., Cotiviti, Inc., IQVIA, Inovalon, Symphony Health, Definitive Healthcare, Truveta, Arcadia Solutions, LLC
b. Key factors that are driving the market growth include rapid expansion of healthcare data volume (EHR, Claims, Wearables), rising demand for Real-World Data (RWD) & Real-World Evidence (RWE), increasing adoption of AI, advanced analytics & cloud platforms, and growing payer focus on cost optimization & risk management.
Share this report with your colleague or friend.
Need a Tailored Report?
Customize this report to your needs — add regions, segments, or data points, with 20% free customization.

ISO 9001:2015 & 27001:2022 Certified
We are GDPR and CCPA compliant! Your transaction & personal information is safe and secure. For more details, please read our privacy policy.
Trusted market insights - try a free sample
See how our reports are structured and why industry leaders rely on Grand View Research. Get a free sample or ask us to tailor this report to your needs.